Distressing low sexual desire is the most common sexual complaint among women in the United States. Despite the prevalence of this condition and others like it, many healthcare providers find the diagnosis and treatment of female sexual disorders elusive. In late 2016, a team of sexual health experts from the International Society for the Study of Women’s Sexual Health met to develop a process of care (POC) to streamline the management of women with hypoactive sexual desire disorder (HSDD). In April 2018, Mayo Clinic Proceedings published the HSDD POC, which is summarized here.
Approximately 10% of women in the United States report low sexual desire that they find distressing.1 Although the prevalence of distressing low sexual desire is highest among women aged 45-64 years, a woman of any age can experience this problem. Low sexual desire adversely affects one’s self-image and intimate partner relationships.2 Hypoactive sexual desire disorder (HSDD), the diagnostic term for acquired distressing low sexual desire, is the most prevalent sexual disorder in U.S. women, yet it remains widely misunderstood and underdiagnosed.1
 Hypoactive sexual desire disorder is defined by the Diagnostic and Statistical Manual of Mental Disorders (DSM) as persistently or recurrently deficient (or absent) sexual fantasies and desire for sexual activity, which causes marked distress or interpersonal difficulty.3 HSDD can be lifelong or acquired, and generalized or situational.4 Healthcare providers (HCPs) need to accurately identify the type of HSDD an individual is experiencing in order to appropriately manage her care.
Hypoactive sexual desire disorder is defined by the Diagnostic and Statistical Manual of Mental Disorders (DSM) as persistently or recurrently deficient (or absent) sexual fantasies and desire for sexual activity, which causes marked distress or interpersonal difficulty.3 HSDD can be lifelong or acquired, and generalized or situational.4 Healthcare providers (HCPs) need to accurately identify the type of HSDD an individual is experiencing in order to appropriately manage her care.
Of note, the DSM-5no longer includes the term hypoactive sexual desire disorder.5 Instead, disorders pertaining to low sexual desire and female arousal disorder are merged into a singular term, female sexual interest and arousal disorder (FSIAD).5 The merging of desire and arousal disorders into one term is not widely endorsed in the sexual health community. In addition, most published research to date in the realm of distressing low sexual desire has used the term HSDD instead of the term FSIAD. From this point forward, this column refers solely to HSDD.
Background
Journal articles first published content on HSDD in the 1970s.1,6 As with past beliefs about depression, HSDD is often incorrectly perceived as a fabricated condition, with no biochemical basis, that is intended for pharmaceutical gain. Current understanding of HSDD is that it is a real condition with various potential contributing causes and profound biopsychosocial ramifications.7-10
Sexual response relies on a balance between excitatory and inhibitory factors.11,12 Known excitatory factors in sexual response include the biochemical compounds dopamine, norepinephrine, oxytocin, and melanocortin, and human emotional connectors such as intimacy, romance, and shared values.11,12 Inhibitory factors include the biochemical compounds serotonin, endocannabinoids, endogenous opioids, and prolactin, and human emotional disconnectors such as relationship conflict, negative stress, and negative beliefs about sex.11,12 In many cases, a combination of inhibitory factors contributes to HSDD.
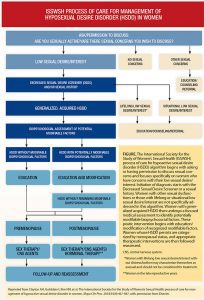
The International Society for the Study of Women’s Sexual Health process of care (POC) for HSDD provides a simplified method for evaluating, diagnosing, and treating female patients with distressing low sexual desire (Figure).13 The HSDD POC encourages use of a biopsychosocial approach to fully understand the unique experiences of individual women with HSDD.4,7,13
Opening the conversation
As with all interactions between patient and HCP, both participants must feel safe and comfortable, especially when discussing sensitive issues such as sexual intimacy. The best way for an HCP to initiate a conversation about sex in a patient encounter is to ask the patient if she is sexually active.14 Next, the HCP can pose a more direct question that allows the patient to tell her story. For example, the HCP can ask her whether she has any concerns about her sexual health that she wants to discuss at the visit. It is helpful to normalize a conversation about sexual health by telling the patient that many women experience challenges in terms of their sexual functioning.
Screening
The Decreased Sexual Desire Screener (DSDS), a validated tool, helps rule out contributing causes to low sexual desire and expedite the proper diagnosis of generalized acquired HSDD.15-16 1The DSDS is designed for patients to self-administer and can be completed in a few minutes.15
If an HCP has an adequate comfort level and has experience in sexual medicine, then the next step is to obtain the patient’s sexual health history. Of importance, the HCP also needs to be unbiasedduring a sexual health interview. The HCP should never make any assumptions—based on a patient’s age, race, religious beliefs, appearance, partnered/marital status, or socioeconomic status—about her sexual orientation, monogamy status, type or frequency of sexual practices, or propensity for masturbatory behavior. If an HCP is not comfortable discussing or managing problems related to sexual dysfunction, then the HCP can validate the patient’s concerns and offer referral to a qualified practitioner.
When I interview patients about their sexual health, I start by reinforcing the confidentiality of our conversation. Next, I make an open-ended statement/request: I understand you have some concerns related to low sex drive. Tell me your story. This statement communicates to the patient that I am comfortable with the topic and want to know her entire experience related to low sexual desire. If time is limited, I say to the patient: I find your concerns valid and worthy of a discussion. Let’s schedule another appointment to focus on these concerns.
Assessment of potentially modifiable factors
As part of the biopsychosocial assessment in the HSDD POC, HCPs should perform a physical examination and order laboratory testing when indicated.13,17 The physical exam, including a full vulvovaginal exam, provides a window into the hormonal status of the woman, among other useful information. In addition, the vulvovaginal exam facilitates an opportunity for the HCP to educate the patient about the anatomic structures of her genitals and sexual health physiology. When appropriate, use of a mirror to identify genital landmarks during an exam can reassure a woman of her urogenital health, as well as empower her to explore erogenous areas during future sex play. I dub this educational opportunity Vagina 101. Many of my patients find this “class” incredibly helpful because they feel uncomfortable or ill equipped to explore their genital anatomy on their own.
Hypoactive sexual desire disorder is a diagnosis of exclusion. Contributing causes of distressing low sexual desire, including cardiovascular, dermatologic, urogynecologic, and endocrine disorders, should be explored and addressed.13 Laboratory testing, including measurement of levels of follicle-stimulating hormone, luteinizing hormone, estradiol, progesterone, testosterone, dihydrotestosterone, and sex hormone-binding globulin, should be considered in appropriate cases.13 In addition, measurement of prolactin and thyroid hormone levels can aid in identification of potential physiologic causes of distressing low sexual desire.13 HCPs should also consider medications that affect sexual functioning—including stimulants, cardiovascular agents, psychotropic medications, opioids, and hormonal agents—that the patient may be using.13, 18
Menopausal status of the woman must be determined in order to properly follow the HSDD POC. In a woman of unknown menopausal status, the Stages of Reproductive Aging Workshop (STRAW + 10) indicates typical changes associated with menopause.19 Once a woman is identified as being pre- or postmenopausal, an HCP may choose the appropriate treatment pathway in the HSDD POC.19
Treatment
After a diagnosis of HSDD has been made, the patient should be offered education about the condition and management of potentially modifiable factors.13 In cases where HSDD persists despite first- and second-line therapies, pharmaceutical intervention and sex therapy may be considered.13 Treatment of HSDD in premenopausal women should include consideration of sex therapy with a certified sex therapist and/or use of central nervous system-acting agents.13 In postmenopausal women with HSDD, use of hormonal therapy should be considered.13
Only one medication, flibanserin, is FDA approved for the treatment of HSDD in premenopausal women. This oral medication has a strong agonistic effect on serotonin 5-HT1A receptors, a weak agonistic effect on dopamine D4 receptors, and an antagonistic effect on 5-HT2A receptors.20 Phase III trials of flibanserin demonstrated statistically significant improvements in sexual desire and satisfying sexual events, as well as a reduction in distress, with active treatment versus placebo after 8 weeks.21 In 2015, Sprout Pharmaceuticals gained FDA approval to launch flibanserin in the U.S.20
Another medication, bremelanotide (BMT), remains under development as an on-demand, injectable, peptide melanocortin receptor agonist.22 Palatin Technologies plans to seek FDA approval for BMT near the end of 2018 for the indication of HSDD in premenopausal women. Results of phase III clinical trials showed statistically significant improvements in sexual desire and reduced distress with this agent.22 In addition, BMT is associated with improvements in sexual arousal, vaginal lubrication, orgasm, and satisfaction—as evidenced by corresponding Female Sexual Function Index domain scores.22,23 Although not FDA approved for use specifically in HSDD, testosterone products and oral bupropion have been used off-label by sexual medicine experts to treat distressing low sexual desire in women.17,24,25
Referral to a certified sex therapist is another highly useful option for treating women with HSDD.13 Sex therapists use various interventions, including behavior therapy, cognitive behavioral therapy, and mindfulness therapy, to treat HSDD.13 Local sex therapists and sexuality educators can be identified on the Society for Sex Therapy & Research website and the American Association of Sexuality Educators Counselors and Therapists website.
Conclusion
Hypoactive sexual desire disorder is the most common sexual dysfunction among U.S. women. Nevertheless, many women with HSDD do not seek or receive appropriate care for their symptoms. The HSDD POC helps guide HCPs in utilizing a biopsychosocial approach to screen, diagnose, and treat women with distressing low sexual desire.13
Brooke M. Faught is a nurse practitioner and the Clinical Director of the Women’s Institute for Sexual Health (WISH), A Division of Urology Associates, in Nashville, Tennessee. She is a Fellow of the International Society for the Study of Women’s Sexual Health (ISSWSH). The author states that she serves as a speaker and an advisory board member for AMAG and as an advisory board member for Symbiomix, Duchesnay, and AMAG.
References
- Shifren JL, Monz BU, Russo PA, et al. Sexual problems and distress in United States women: prevalence and correlates. Obstet Gynecol. 2008;112(5):970-978.
- Kingsberg SA. Attitudinal survey of women living with low sexual desire. J Womens Health. 2014;23(10):817-823.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Text Revision. Washington, DC: American Psychiatric Association; 2000.
- Parish SJ, Goldstein AT, Goldstein SW, et al. Toward a more evidence-based nosology and nomenclature for female sexual dysfunctions—part II. J Sex Med. 2016;13(12):1888-1906.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
- Kaplan HS. Hypoactive sexual desire. J Sex Marital Ther. 1977;3(1):3-9.
- Althof SE, Leiblum SR, Chevret-Measson M, et al. Psychological and interpersonal dimensions of sexual function and dysfunction. J Sex Med. 2005;2(6):793-800.
- Leiblum SR, Koochaki PE, Rodenberg CA, et al. Hypoactive sexual desire disorder in postmenopausal women: US results from the Women’s International Study of Health and Sexuality (WISHeS). Menopause. 2006;13(1):46-56.
- Dennerstein L, Koochaki P, Barton I, Graziottin A. Hypoactive sexual desire disorder in menopausal women: a survey of Western European women. J Sex Med. 2006;3(2):212-222.
- Kingsberg SA, Clayton AH, Pfaus JG. The female sexual response: current models, neurobiological underpinnings and agents currently approved or under investigation for the treatment of hypoactive sexual desire disorder. CNS Drugs. 2015;29(11):915-933.
- Bancroft J, Graham CA, Janssen E, Sanders SA. The dual control model: current status and future directions. J Sex Res. 2009;46(2-3):121-142.
- Perelman MA. The Sexual Tipping Point: a mind/body model for sexual medicine. J Sex Med. 2009;6(3):629-632.
- Clayton AH, Goldstein I, Kim NN, et al. The International Society for the Study of Women’s Sexual Health process of care for management of hypoactive sexual desire disorder in women. Mayo Clin Proc. 2018;93(4):467-487.
- Kingsberg S. Just ask! Talking to patients about sexual function. Sex Reprod Menopause. 2004;2(4):199-203.
- Goldfischer E, Clayton AH, Goldstein I, Pyke R. Decreased Sexual Desire Screener (DSDS) for diagnosis of hypoactive sexual desire disorder in women. J Sex Med. 2009;6:10.
- Clayton AH, Goldfischer E, Goldstein I, et al. Validity of the decreased sexual desire screener for diagnosing hypoactive sexual desire disorder. J Sex Marital Ther. 2013;39(2):132-143.
- Goldstein I, Kim NN, Clayton AH, et al. Hypoactive sexual desire disorder: International Society for the Study of Women’s Sexual Health (ISSWSH) expert consensus panel review. Mayo Clin Proc. 2017;92(1):114-128.
- Buster JE. Managing female sexual dysfunction. Fertil Steril. 2013;100(4):905-915.
- Kirana PS, Papaharitou S, Athanasiadis L, et al. A conceptual framework for the evolution of sexual medicine and a model for the development of alternative sexual health services: 10-year experience of the center for sexual and reproductive health. J Sex Med. 2009;6(9):2405-2416.
- Borsini F, Evans K, Jason K, et al. Pharmacology of flibanserin. CNS Drug Rev. 2002;8(2):117-142.
- Katz M, DeRogatis LR, Ackerman R, et al. Efficacy of flibanserin in women with hypoactive sexual desire disorder: results from the BEGONIA trial. J Sex Med. 2013;10(7):1807-1815.
- Kingsberg S, Lucas J, Jordan R, Spana C. Efficacy of bremelanotide for hypoactive sexual desire disorder (Reconnect Study). J Sex Med. 2017;14(5):e335.
- Rosen C, Brown J, Heiman S, et al. The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther. 2000;26(2):191-208.
- Davis SR, Worsley R, Miller KK, et al. Androgens and female sexual function and dysfunction—findings from the Fourth International Consultation of Sexual Medicine. J Sex Med. 2016;13(2):168-178.
- Segraves RT, Clayton A, Croft H, et al. Bupropion sustained release for the treatment of hypoactive sexual desire disorder in premenopausal women. J Clin Psychopharmacol. 2004;24(3):339-342.

