Women with long or irregular periods are known to have a higher risk of type 2 diabetes and heart disease, but researchers found these women may also be at risk for nonalcoholic fatty liver disease (NAFLD), according to a new study published in the Endocrine Society’s Journal of Clinical Endocrinology and Metabolism.
The researchers at the Center for Cohort Studies, Total Healthcare Center, Kangbuk Samsung Hospital, Sungkyunkwan University School of Medicine in Seoul, South Korea, performed a cross-sectional analysis of more than 70k women younger than 40 years of age and found that those with long or irregular menstrual cycles were at a 22% greater risk of developing NAFLD.
Nearly 1 in 4 U.S. females with NAFLD
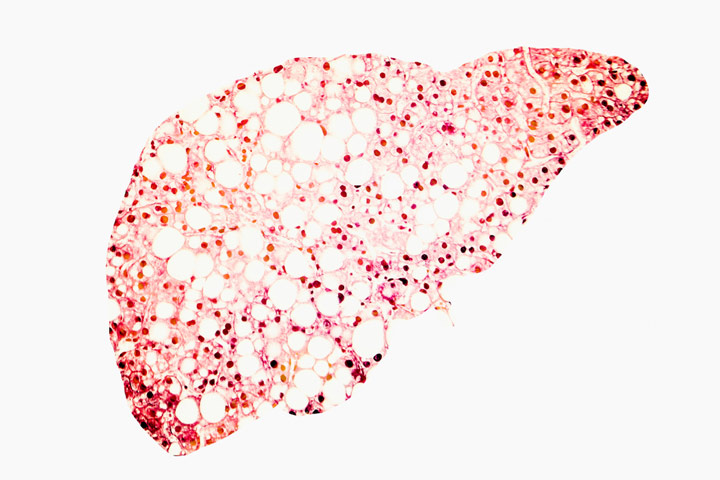
NAFLD is a chronic disease in which excess fat builds up in the liver, a fat buildup not caused by heavy alcohol use. NAFLD represents a spectrum of liver diseases that range from simple steatosis to nonalcoholic steatohepatitis (NASH), cirrhosis, and hepatocellular carcinoma. It has been clearly demonstrated in previous studies that NAFLD is associated with an increased risk of cardiovascular disease (CVD) independent of other CVD risk factors such as obesity and diabetes. In fact, CVD is the most frequent cause of death among patients with NAFLD (Athyros, 2017).
Arshad and colleagues found that most recent prevalence of NAFLD among female adults in the United States was slightly over 24% and further, that the average age of the female population with NAFLD has decreased over time. The prevalence of NAFLD among younger women 20 to 44 years of age has increased from 11% to 17% (Arshad et al,2018).
Well-powered, 4+ years of follow-up
Among the study’s 72,092 premenopausal Korean women under the age of 40, 7.1% had NAFLD at baseline and 27.7% had long or irregular menstrual cycles defined as menstrual cycles of 40 days or longer or too irregular to estimate. The study’s final cohort underwent annual exams at a health center in Seoul and Suwon, South Korea. Exclusion criteria included a history of liver disease, hepatitis B or C, higher alcohol consumption, and abnormal thyroid functioning. NAFLD diagnosis was based on hepatic steatosis identified on abdominal ultrasonography performed by radiologists.
During a median follow-up of 4.4 years, incident NAFLD occurred in 8.9% of the women. In the investigators’ analyses, long or irregular menstrual cycles were positively associated with prevalent NAFLD. Specifically, the risk for NAFLD among those with long or irregular menstrual cycles was 22% greater than that observed for the reference group after adjustment for age, BMI, insulin resistance, and other confounders (HR, 1.22; 955 CI, 1.14-1.31).
Not explained by insulin resistance, obesity
In a time-dependent analysis, this relationship only strengthened the more irregular a cycle was, the authors explained.
In a subgroup analysis of women with a homeostatic model assessment of insulin resistance (HOMA-IR) less than 2.5 — indicating less insulin resistance — these associations were weakened but were still significantly high: women with 31- to 39-day and ≥40-day irregular menstrual cycles saw an 18% and 27% higher risk for developing NAFLD, respectively.
“This suggests that insulin resistance, which has been posited to contribute to the association between [polycystic ovary syndrome] and NAFLD, does not fully explain the association between long or irregular menstrual cycles and NAFLD demonstrated in our study,” the researchers pointed out.
“This link was not explained by obesity,” they continued. “Previous studies have shown that long or irregular menstrual cycles are associated with type 2 diabetes and cardiovascular disease, but our study is the first to find a link between long or irregular menstrual cycles and NAFLD.”
Potential hypotheses
The group explained that while the mechanisms underlying the association between long or irregular menstrual cycles and NAFLD have yet to be determined, some possible explanations could be estrogen exposure, androgen excess, and hypogonadotropic hypogonadism.
“Importantly, our results indicate that menstrual irregularity, which is easier to diagnose and usually presents earlier than PCOS, highlights the possibility of identifying premenopausal women at risk of developing NAFLD,” the authorswrote.
A diagnostic clue for NAFLD
NAFLD causes no symptoms in most cases and no drug treatment has yet been approved for it by the Food and Drug Administration. As such, the study’s findings may serve as invaluable clinical clue for women’s healthcare providers to consider NAFLD and counsel young women with long or irregular menstrual cycles about lifestyle changes that can reduce their risk of NAFLD as well as other cardiometabolic diseases.
Find the complete study, “Long or Irregular Menstrual Cycles and Risk of Prevalent and Incident Non-Alcoholic Fatty Liver Disease,” at https://academic.oup.com/jcem/advance-article-abstract/doi/10.1210/clinem/dgac068/6539695?redirectedFrom=fulltext