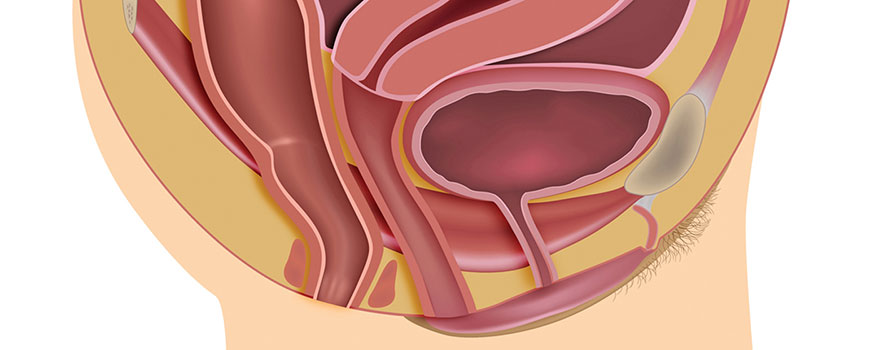
Pelvic organ prolapse (POP) is a prevalent condition that can cause uncomfortable sensations of vaginal bulging, painful intercourse, and even stress urinary incontinence. This article presents a simple, evidence-based approach to diagnosing and managing POP that women’s healthcare providers can implement.
Pelvic organ prolapse (POP) is a common condition that occurs when one or more pelvic structures—the bladder, the urethra, the uterus, or the rectum—deviate from their normal anatomic position and bulge against the vaginal vault.1 Sometimes the prolapse is so severe that the affected area protrudes through the vaginal opening. The underlying cause of POP is a weakening of the pelvic floor muscles (PFMs) and fascia that support the pelvic organs.2
Risk factors
Loss of PFM tone may be caused by a variety of factors. One common risk factor for POP is multiple vaginal deliveries, particularly in those women who have experienced prolonged labor, instrumented delivery, and/or delivery of infants weighing more than 9 lb. In fact, women who have delivered vaginally, compared with those who have undergone cesarean section, have twice the risk of developing symptomatic POP.3 Women who have had pelvic floor trauma during childbirth or pelvic surgery such as hysterectomy are also at increased risk for POP.
Other risk factors for POP include conditions that increase intra-abdominal pressure such as chronic constipation, chronic cough, and work involving prolonged heavy lifting.3,4 Still other contributing factors are excess body weight, aging, menopause (related to loss of collagen), genetic predisposition, prolonged standing, and activities that involve jumping (e.g., trampoline use).5 Overweight and obesity are particularly strong risk factors: Studies have shown that the risk for symptomatic POP rises 3% with each unit increase of body mass index (BMI), and that women whose BMIs exceed 25 kg/m2, as compared with women whose BMIs are below 25, are twice as likely to develop POP.3,4 Health conditions that may disrupt pelvic neuromuscular function—and therefore increase the risk for developing POP—include multiple sclerosis, neuromuscular injuries related to childbearing, and spinal cord injury.5-7
Clinical picture
Many women with mild POP are asymptomatic. A woman with symptomatic POP may report feeling pressure or fullness in the pelvis, a pulling sensation in the groin or lower back, or vaginal bulging—all of which may ease up when she lies flat. She may describe a feeling that something is falling out of the vagina or even have a visible bulge from the vagina. Either way, she may experience vaginal pain or discomfort, particularly when having sex.4,6
Urinary symptoms of POP may include stress urinary incontinence (SUI), difficulty voiding, a sensation that one cannot empty the bladder completely, urinary frequency, urinary urgency, or nocturia. With some forms of POP, urinary symptoms are actually masked. Bowel symptoms of POP may include pain with defecation, fecal incontinence, or other types of defecatory dysfunction. A patient with a rectocele may report that she needs to press between the vagina and rectum to help her defecate.
The healthcare provider (HCP) must take a thorough history regarding these symptoms, as well as a detailed gynecologic, obstetric, sexual, and surgical history, to determine contributing factors. In addition, the HCP needs to identify chronic health conditions or situations that could be contributing to longer-than-average periods of elevated intra-abdominal pressure. These include chronic constipation and smoking or respiratory conditions that cause chronic cough.1,4 As part of the behavioral history, the HCP needs to ask about the patient’s exercise regimen (e.g., Does she lift weights? Does she do jumping jacks or use a trampoline?), whether the patient has gained weight recently, and whether the patient’s occupation may require her to perform heavy lifting or stand for long periods of time.
Physical examination
Because many patients have more than one type of prolapse, the HCP needs to examine each area of potential involvement within the vaginal vault separately. Performing each component of the pelvic exam with an individual focus results in greater accuracy of diagnosis.
Grading system
Various grading systems are available to determine the severity of POP based on physical examination. In this article, the authors use the Baden-Walker Halfway Scoring System, which assigns these gradations of severity:
• Grade 0: no prolapse;
• Grade 1: the lowest part of protrusion extends halfway to the hymen;
• Grade 2: the lowest part of protrusion extends to the hymen;
• Grade 3: the lowest part of protrusion extends halfway past the hymen; or
• Grade 4: the greatest degree of protrusion is observed.8, 9
The other commonly used grading system, albeit more complex than the Baden-Walker system, is the Pelvic Organ Prolapse Quantification (POP-Q) system.10
Inspection of external genitalia
Once the required equipment is assembled and available and the patient is placed in the lithotomy position, the exam begins with an inspection of the external genitalia.1,9,11 In a woman with normal findings, the vaginal introitus may be small or wide, depending on her sexual status, and hymenal remnants may be observed. Abnormal findings may include dry tissue, bruising, lesions, discharge,or prolapsed vaginal tissue. The introitus may gape open if vaginal vault/uterine prolapse is present. If prolapse is observed on inspection, the HCP should check for ulcerations. In severe POP, the prolapse may be observed on inspection even if the patient has not been asked to strain.
Speculum examination
During the speculum examination, the HCP inspects the vaginal mucosa for symmetry, atrophy, and any other abnormalities such as ulcerations or discharge that might explain the presence of symptoms.9 First, the speculum is placed into the vaginal vault and the cervix is inspected. Next, as the speculum is slowly removed, the vaginal mucosa is observed for any abnormalities such as abrasions or descent of the vaginal apex while the patient is asked to perform the Valsalva maneuver.9 The extent to which the cervix or the vaginal vault follows the speculum through and out of the vagina is noted.1
Next the HCP inserts the posterior blade of the speculum into the vagina, applying gentle pressure first to the posterior wall while asking the woman to perform the Valsalva maneuver to look for the extent of anterior compartment protrusion at the lowest point of the descent. The HCP then rotates the blade, applying gentle pressure to the anterior vaginal wall to determine if any prolapse is present in the posterior compartment and to what degree—based on the Baden-Walker system (Table).9,11
The patient may be concerned about leaking urine or stool when asked to bear down during these exams. The HCP should provide reassurance to her and equip the room with waterproof pads and hygiene products such as tissue or unscented, hypoallergenic moist cloths for cleaning as needed.
Bimanual examination
A bimanual exam is performed to evaluate the size and shape of the uterus and ovaries and to check for the presence of abdominal masses. The uterus should feel smooth and round and move slightly with manipulation. The ovaries, if palpable, should be no larger than the size of an almond. All organs should be non-tender on examination. The bimanual exam can help identify other pathologies that might be contributing to the chief complain of pelvic pressure and other reported symptoms.
During this exam component, the HCP can assess the adequacy of the patient’s vaginal muscle tone in supporting the pelvic organs by having her contract the PFMs. While performing this assessment, the HCP needs to determine whether voluntary or involuntary contractions are occurring, whether muscles remain in a contracted state, and whether the PFMs do not contract at all, even when the patient is asked to contract them.9
Examination while patient is standing
The inspection exam with Valsalva straining is repeated while the patient is standing. This exam provides the best estimation of the extent of prolapse as it relates to normal daily activities.9 Depending on the patient’s symptoms, the HCP may also perform a rectal exam with the patient standing to check for an enterocele as the cause of the symptoms.9 If the small bowel is involved, it will be palpable in the cul-de-sac.
Differential diagnoses
Differential diagnoses to consider when assessing a woman for POP include adnexal, uterine, and other genital tract masses that may cause symptoms similar to those of POP; and urinary tract infection (UTI).9 If the patient has urinary symptoms, a urinalysis is done to evaluate for UTI.9
Treatment
Treatment for POP is based on severity of the prolapse and the patient’s preferences, health, and symptoms. Conservative options, though associated with few adverse effects and cost-effective, tend to work only for milder forms of POP and require a high level of commitment from the patient. Examples of conservative options are behavior modification (e.g., weight-loss diet, smoking cessation), PFM strengthening, and pessaries.9,12 Goals of conservative therapy are to improve symptoms, reduce POP progression, and delay or avoid surgery.
Pelvic floor muscle strengthening
If POP is grade 2 or lower, PFM strengthening, including Kegel exercises, can improve symptoms of pelvic pain, vaginal pressure or bulging, and SUI.12,13 Evidence regarding the efficacy of PFM strengthening in improving POP symptoms and degree is limited, but recent studies have shown significant improvement with this approach.13,14 For a patient who wants to learn to perform Kegel exercises, she should start slowly and increase gradually, with the goal of performing 10 contractions held for 10 seconds each, 2-3 times daily.12,15
Pessary
The pessary, a flexible plastic or medical-grade silicone device that comes in a variety of sizes and shapes, can be used to treat any grade of POP.1 It is inserted into the vaginal vault to support weakened PFMs and prevent bulging. The pessary is a good choice for a woman with bothersome POP symptoms who is not a candidate for or does not desire surgery. The pessary may be used for temporary symptomatic relief while awaiting surgery. Potential adverse effects of the pessary include changes in voiding patterns, vaginal irritation, and vaginal ulcers or excoriations.12 Pessary use is avoided if a woman has a large vaginal outlet or a short vagina, and it may be challenging if a woman cannot insert or withdraw the device on her own.15 A woman may receive assistance from a home health nurse or return to the office at regular intervals to have the device removed, cleaned, and replaced, although the frequency with which she needs to return for pessary followup or periodic cleaning has not been established.12
Surgery
Surgery is an option for a woman whose symptoms are adversely affecting her quality of life. Several different surgical procedures are available. Colporrhaphy is done to repair the anterior or posterior vaginal wall in a woman with cystocele or rectocele. The affected organ (i.e., the bladder or rectum) is moved back into normal position and the affected vaginal wall is tightened to better support the organ. Surgical implantation of transvaginal mesh for correcting POP has become more common because of the higher rates of success compared with traditional colporrhaphy.16 However, postoperative complications (e.g., mesh erosion, operative site pain, painful urination) may arise, and longterm efficacy of the treatment has not been established.16-19
Patient counseling
If conservative management is desired and the grade of POP is 2 or lower, HCPs should counsel patients with regard to performing Kegel exercises and on behavior modification strategies, which include weight loss; smoking cessation; and avoidance of straining with bowel movements, prolonged standing, lifting, and exercise involving jumping. Patients need to know that conservative measures can be quite helpful in reducing POP progression. Patients also need to understand the risks of surgery, which include incontinence and erosion or contraction of the mesh.17
Referral
Need for referral depends on the plan for POP management and the HCP’s skills in diagnosing and managing the condition. If POP is only mildly bothersome, the HCP may choose to begin PFM strengthening and fit the patient with a pessary.13 Referral to a specialist is made if the diagnosis is uncertain or if surgical evaluation is desired. In addition, patients may be referred to a pelvic floor physical therapist for intense and focused assistance with PFM strengthening to relieve symptoms.
Conclusion
Pelvic organ prolapse can be an embarrassing, bothersome problem for women. HCPs need to know the risk factors and symptoms associated with POP, how to evaluate for the condition on physical exam,and the various treatment options that are available. Treatment choice is based on symptom severity and patient preference. Referral to a specialist is recommended when factors related to evaluation and treatment begin to exceed an HCP’s scope of practice.
Brittany S. Nutt is a DNP graduate of Texas Woman’s University in Dallas and a Women’s Health Nurse Practitioner in the United States Air Force. Susan Chaney is Master of Science Program Coordinator and Professor and Catherine Hill is Clinical Faculty, both at Texas Woman’s University in Dallas. Catherine Hill is also Managing Partner of Texas Nurse Practitioner Associates, LLP, in Dallas. The authors state that they do not have a financial interest in or other relationship with any commercial product named in this article.
References
1. Kuncharapu I, Majeroni BA, Johnson DW. Pelvic organ prolapse. Am Fam Physician. 2010;81(9):1111-1117.
2. American College of Obstetricians and Gynecologists. Frequently Asked Questions: Gynecologic Problems. FAQ012. Pelvic Support Problems. May 2011.
3. Gyhagen M, Bullarbo M, Neilsen TF, Milsom I. Prevalence and risk factors for pelvic organ prolapse 20 years after childbirth: a national cohort study in a singleton primiparae after vaginal or caesarean delivery. BJOG. 2013;120(2):152-160.
4. Rogers RG, Fashokun TB. An overview of the epidemiology, risk factors, clinical manifestations, and management of pelvic organ prolapse. UpToDate. Last updated February 19, 2015.
5. Lukanovic A, Drazic K. Risk factors for vaginal prolapse after hysterectomy. Int J Gynaecol Obstet. 2010;110(1):27-30.
6. Handa VL. Urinary incontinence and pelvic organ prolapse associated with pregnancy and childbirth. UpToDate. Last updated May 27, 2015.
7. Mahajan ST, James R, Frasure H. Pelvic floor disorders and multiple sclerosis: are patients satisfied with their care? Int J MS Care. 2014;16(1):20-25.
8. ACOG Practice Bulletin No. 85: Pelvic organ prolapse. Obstet Gynecol. 2007;110(3):717-729.
9. Fashokun TB, Rogers RG. Pelvic organ prolapse in women: diagnostic evaluation. UpToDate. Last updated June 15, 2015.
10. Persu C, Chapple CR, Cauni V, et al. Pelvic Organ Prolapse Quantification System (POP-Q) – a new era in pelvic prolapse staging. J Med Life. 2011;4(1):75-81.
11. Seidel HM, Ball JW, Dains JE, Benedict GW. Mosby’s Guide to Physical Examination. Fifth Edition. St. Louis, MO: Mosby; 2003.
12. Hagen S, Thakar R. Conservative management of pelvic organ prolapse. Obstet Gynaecol Reprod Med. 2012;22(5):118-122.
13. Braekken IH, Majida M, Engh ME, Bo K. Can pelvic floor muscle training reverse pelvic organ prolapse and reduce prolapse symptoms? An assessor-blinded, randomized, controlled trial. Am J Obstet Gynecol. 2010;203(2):170.e1-7.
14. Hagen S, Stark D, Glazener C, et al. Individualised pelvic floor muscle training in women with pelvic organ prolapse (POPPY): a multicentre randomized controlled trial. Lancet, 2013;383(9919):796-806.
15. Choi KH, Hong JY. Management of pelvic organ prolapse. Korean J Urol. 2014;55(11):693-702.
16. Turgal M, Sivaslioglu A, Yildiz A, Dolen I. Anatomical and functional assessment of anterior colporrhaphy versus polypropylene mesh surgery in cystocele treatment. Eur J Obstet Gynaecol Reprod Biol. 2013;170(2):555-558.
17. Dietz HP, Hankins KJ, Wong V. The natural history of cystocele recurrence. Int Urogynecol J. 2014;25(8): 1053-1057.
18. Walter JE; Urogynaecology Committee, Lovatsis D, et al; Society of Obstetricians and Gynaecologists of Canada. Transvaginal mesh procedures for pelvic organ prolapse. J Obstet Gynaecol Can. 2011;33(2):168-174.
19. Altman D, Vayrynen T, Axelsen S, Falconer C; Nordic Transvaginal Mesh Group. Anterior colporrhaphy versus transvaginal mesh for pelvic-organ prolapse. N Engl J Med. 2013;364(19): 1826-1836.