Advanced practice providers (APPs) may experience burnout threats in their careers at any time.1 Burnout is a problem that not only threatens the health and well-being of APPs but also significantly impacts productivity, job retention, and ultimately the quality of patient care.2 Work-related burnout syndrome has hit epidemic levels with rates that are an evidence-based public health problem.3 Clinicians with burnout syndrome feel emotional exhaustion, depersonalization, and lower personal accomplishment continuously caused by stressors from their environment.4
The rising concern of burnout among APPs has prompted a need for a closer study and strategies to address the problem. In one study of burnout among nurse practitioners in a primary care practice environment, caring for women’s sexual and reproductive health was considered an especially sensitive area and exposure to higher risk factors presented a high level of burnout syndrome for those APPs practicing in women’s health.5 Since early 2020, like all APPs, those in women’s health experienced inadequate staffing, challenging schedules, increased job demands, higher patient acuity, and other work factors in the midst of the Covid pandemic. These concerns brought attention to healthcare providers’ wellbeing, with efforts and strategies targeted to reduce burnout. One such strategy that has been demonstrated to significantly improve stress and burnout in healthcare providers is the use of mobile-based mindfulness meditation.6 A study of pharmacy students found that using the mobile app Headspace for a minimum of 10 minutes per day for a total of 4 weeks reduced perceived stress and increased mindfulness and mental wellbeing, both positively promoting the participants’ healthy lifestyle behaviors.7
Project purpose
The nursing renewal center at an urban-based tertiary hospital provided a well-focused program including a break room, massage room, group fitness including Yoga and Zumba, and instructor-guided mindfulness classes. However, staff members had difficulty leaving their unit to attend these prescheduled 1-hour classes. Therefore, an alternative stress reduction method was explored. The purpose of this evidence-based quality improvement (QI) project was to investigate the effect of mobile-based mindfulness meditation on burnout and to demonstrate an improved burnout rate in APPs in the Women’s Health Department over 12 weeks.
Description of setting and population
The QI project was conducted in the Women’s Health Department within a Northeastern urban-based, tertiary academic health center. The project population consisted of APPs in the women’s health inpatient units. The department had 20 APPs including six certified nurse midwives, two physician assistants, and 12 nurse practitioners delivering care in six areas of women’s health.
Description of quality improvement project
The project used a voiced-guided mindfulness meditation application named Headspace as an intervention. Prior to implementing this project, all APPs received an email invitation to complete a demographic survey through the REDCap database, and instructions to download the Headspace application from their own mobile device. After installing and opening the application, participants created an account to select between 3 and 10 minutes meditation options daily. For this project, all participants utilized the free sessions for 12 weeks and set up a reminder to receive notifications to practice mindfulness daily. There was no obligation to purchase any additional sessions in the application. This project did not set up a tracking method to monitor how often they used Headspace or practiced mindfulness, but the project leader sent emails weekly to remind them to practice in addition to the daily reminder from the Headspace application. Participants were encouraged to practice meditation daily for a minimum of 5 minutes. All participants received another email invitation link through Mind-Garden, which publishes many psychological assessments, for the pre- intervention burnout survey. Instruction and supportive information for participants regarding where and how to seek help was included in the first survey.
Methods to evaluate outcomes
In this project, the burnout scores were measured before and after the 12-week intervention in the same participants. Maslach Burnout Inventory-Human Services Survey (MBI-HSS) was used. This instrument includes 22 items and has been established as a validated and reliable tool to evaluate the prevalence of burnout measured in jobs within human services.8 The instrument has been identified in three dimensions to measure emotional exhaustion (EE), depersonalization (DP), and personal accomplishment (PA) to assess burnout. The survey addressed these three variables EE, DP, and PA with accomplishment from never (0) to every day (6). This project was reviewed and determined to qualify as quality improvement by the University of Pennsylvania’s Institutional Review Board.
Outcomes
Twenty participants were initially recruited, and 18 completed pre- and post-intervention surveys. This represented a 90% participant rate. The sample was exclusively female (100%), predominantly White (72%), Master of Science in Nursing educated (83%), and Doctor of Nursing Practice (DNP) educated (17.6%). The mean age was 41.6 years (standard deviation [SD] = 10.1), with a range of 28 to 67 years. The mean number of years of experience as an APP was 10.0 (SD = 6.4), with a range of 1.5 years to 22 years.
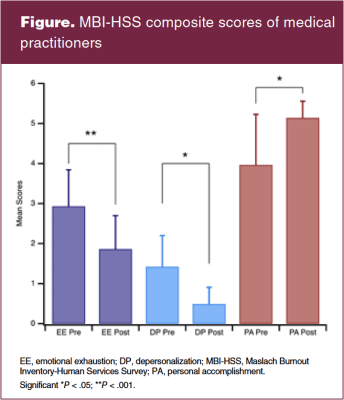
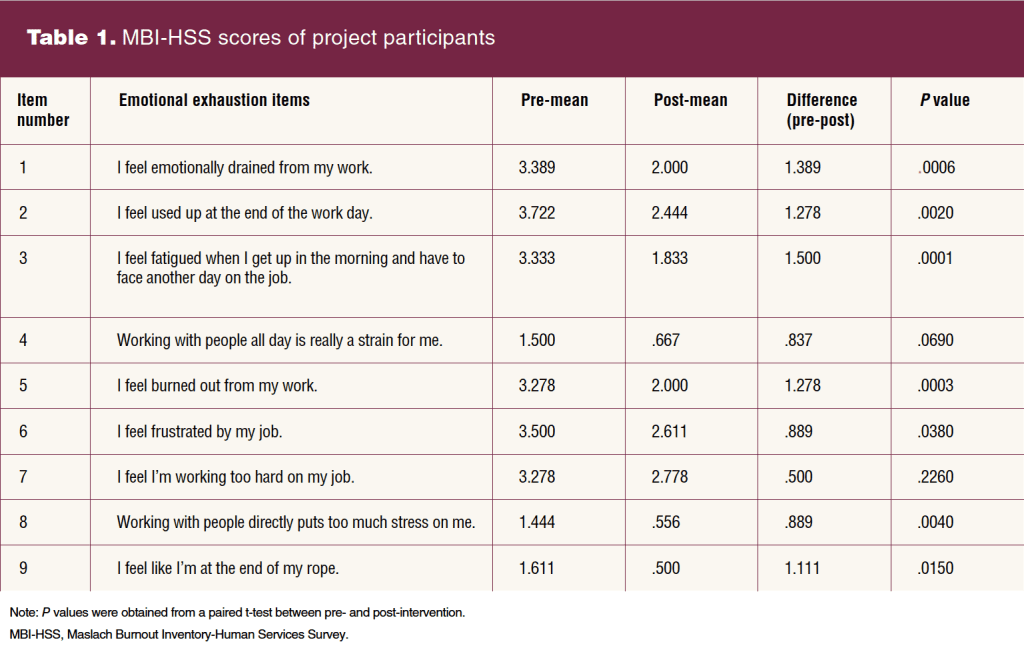
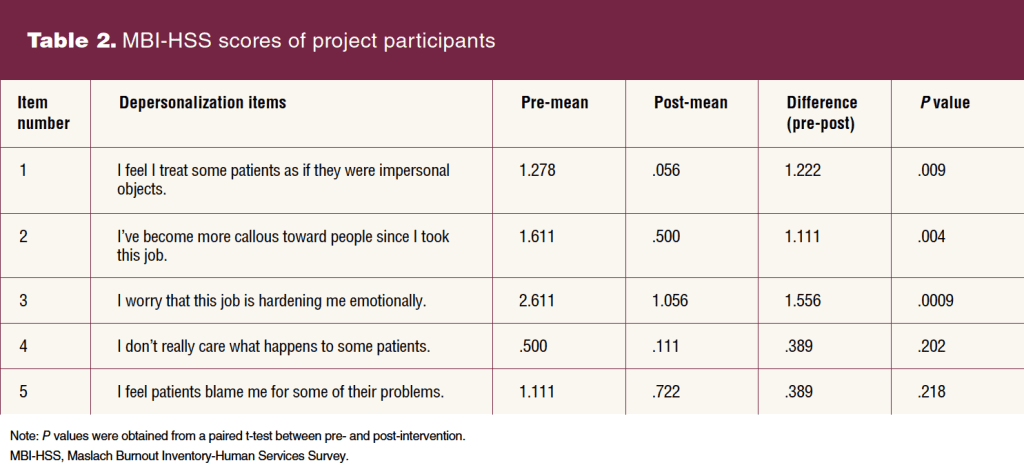
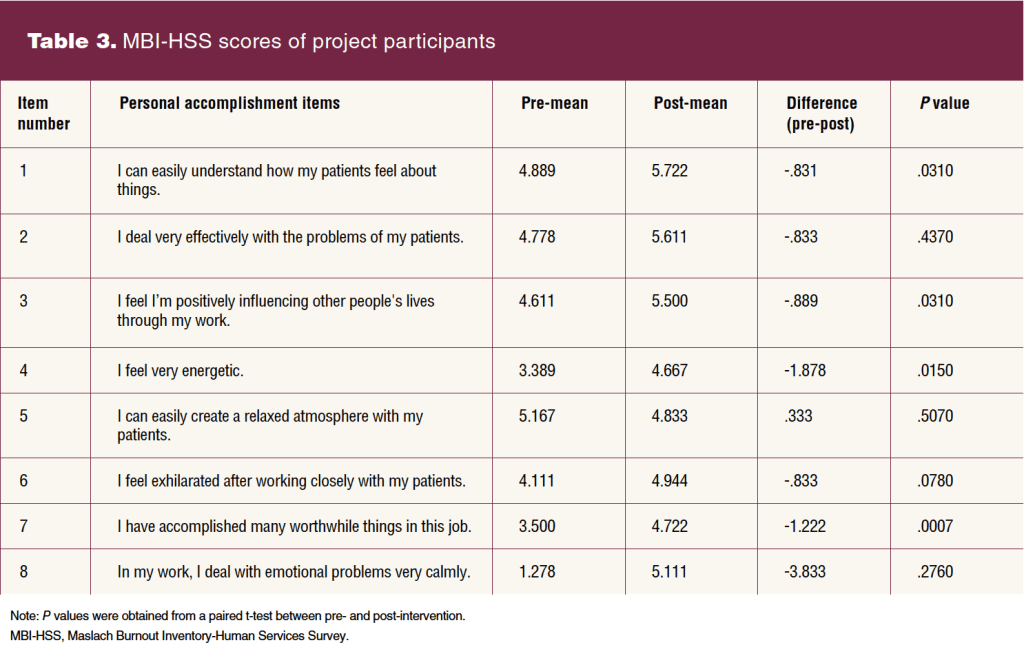
Higher scores on the EE and DP subscales indicated a higher burnout symptom weight, and lower scores on the PA subscale indicated a higher burnout symptom burden. Pre- and post-intervention scores of EE, DP, and PA are included in Tables 1, 2, 3, respectively. Composite scores can be found in the Figure.
Discussion and implications for practice
The findings from the QI project suggested that a mindfulness meditation program reduced burnout among the participants. Many organizations focus significantly on the patient experience and are not focusing on the under-recognized burnout of APPs.9 Organizations could choose to prioritize staff wellbeing to maintain professional strength and provide high quality and safety for patient care.
Successful implementation of an innovative DNP project and subsequent sustainability were essential to this project. The project sustainability was maintained by collaborating with department directors, managers, and APPs, having meetings weekly, and using the most effective and efficient communication regarding the project. APPs continue to receive daily automated text message reminders from the Headspace application. The project leader launched a mobile-based meditation Wellness Champion. To reach the highest level of engagement, all the champions were invited to share their success stories in meetings. The outstanding APPs who went above and beyond on challenges could earn a Super Star “High Five” created by an internal website in the organization. The project leader used a secret Santa gift exchange opportunity to give each APP a personalized coffee mug printed with meditation pictures and inspirational meditation words to remind and encourage them to practice meditation daily. The goal was to not only sustain the project but also more importantly to promote healthy APPs, because promoting physical and mental health for staff had a direct correlation to high-quality patient care. Future plans could include applying for grants to replicate and expand the project.
Conclusion
Some limitations were associated with this QI project. First, the project leader did not have a standardized methodology to track participants. All the participants were recruited into the intervention regardless of their previous use of mindfulness meditation. Second, the project was implemented and completed during the Covid pandemic when burnout scores may be increased compared to a non-pandemic period. Finally, the study had a small number of participants.
In conclusion, the QI project utilized the Headspace application as an intervention to allow APPs to reduce stress and burnout daily at an APP’s own designated time and place. The project outcomes demonstrated a significant improvement on burnout and stress reduction.
Wei Zhou is a women’s health nurse practitioner at the Hospital of the University of Pennsylvania in Philadelphia. Anne E. Lara is an adjunct professor at the College of Health Professions, University of Wilmington, in Wilmington, Delaware. Bridget Howard is the manager of Advanced Practice Providers Women’s Health at the Hospital of the University of Pennsylvania. The authors have no actual or potential conflicts of interest in relation to the contents of this article.
Womens Healthcare. 2023;11(3):45-48. doi: 10.51256/WHC062345
References
1 Harris DA, Haskell J, Cooper E, et al. Estimating the association between burnout and electronic health record-related stress among advanced practice registered nurses. Appl Nurs Res. 2018;43:36-41.
2 Hoff T, Carabetta S, Collinson GE. Satisfaction, burnout, and turnover among nurse practitioners and physician assistants: a review of the empirical literature. Med Care Res Rev. 2019;76(1):3-31.
3 Friganovic A, Selic P, Ilic B, Sedic B. Stress and burnout syndrome and their associations with coping and job satisfaction in critical care nurses: a literature review. Pychiatr Danub. 2019;31(suppl 1):21-31.
4 de la Fuente J, Lahortiga-Ramos F, Laspra-Solís C, et al. A structural equation model of achievement emotions, coping strategies and engagement-burnout in undergraduate students: a possible underlying mechanism in facets of perfectionism. Int J Environ Res Public Health. 2020;17(6):2106.
5 Abraham CM, Zheng K, Norful AA, et al. Primary care practice environment and burnout among nurse practitioners. J Nurse Pract. 2021;17(2):157-162.
6 Fendel JC, Burkle JJ, Goritz AS. Mindfulness-based interventions to reduce burnout and stress in physicians: a systematic review and meta-analysis. Acad Med. 2021;96(5):751-764.
7 Zollars I, Poirier TI, Pailden J. Effects of mindfulness meditation on mindfulness, mental well-being, and perceived stress. Curr Pharm Teach Learn. 2019;11(10):1022-1028.
8 Mukherjee S, Tennant A, Beresford B. Measuring burnout in pediatric oncology staff: should we be using the Maslach Burnout Inventory? J Pediatr Oncol Nurs. 2020;37(1):55-64.
9 Bianchini C, Copeland D. The use of mindfulness-based interventions to mitigate stress and burnout in nurses. J Nurses Prof Dev. 2021;37(2):101-106.