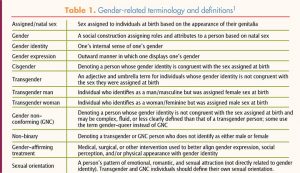
The National Association of Nurse Practitioners in Women’s Health (NPWH) affirms each individual’s right to quality, evidence-based sexual and reproductive healthcare and encourages each individual to strive for a healthy self-concept of sexuality and gender identity. Although NPWH has historically focused on the care of cisgender women, we recognize the importance of providing quality sexual and reproductive healthcare to all individuals, regardless of gender identity. Table 1 provides gender identity-related terminology and definitions.1
 NPWH supports initiatives to address the healthcare needs of transgender and gender non-conforming (GNC) individuals and the implementation of policies and strategies to reduce barriers to inclusive, quality healthcare for these populations. As an organization, NPWH opposes all forms of discrimination against individuals based on sexual orientation, gender expression, or gender identity and urges nurse practitioners (NPs) to speak out against discrimination or victimization of transgender and GNC individuals.
NPWH supports initiatives to address the healthcare needs of transgender and gender non-conforming (GNC) individuals and the implementation of policies and strategies to reduce barriers to inclusive, quality healthcare for these populations. As an organization, NPWH opposes all forms of discrimination against individuals based on sexual orientation, gender expression, or gender identity and urges nurse practitioners (NPs) to speak out against discrimination or victimization of transgender and GNC individuals.
NPWH encourages all NPs who provide sexual and reproductive healthcare to seek out learning opportunities to improve their ability to provide evidence-based, culturally competent care for transgender and GNC individuals. NPWH supports the role of NPs in providing gender-affirming hormone therapy and pre- and post gender-affirming surgery care for individuals who desire such treatment.
NPWH will provide leadership in these areas by offering educational opportunities for NPs and by collaborating with other healthcare organizations that specialize in the care of transgender and GNC individuals. NPWH will also collaborate with other organizations and agencies to develop policies and support research that promotes inclusive, quality, evidence-based care for transgender and GNC individuals.
Background
At the present time, an insufficient number of healthcare providers (HCPs) are adequately prepared and willing to provide care that addresses the unique health concerns of transgender and GNC individuals. Many HCPs report feeling undertrained and ill equipped to care for these populations. Education for NPs and other HCPs has not adequately addressed the health disparities and healthcare needs of transgender and GNC individuals or the provision of culturally competent care for these populations.2

Many transgender individuals seek medical and/or surgical treatments to better align their physical appearance, their gender expression, and social perception with their gender identity. In the 2015 U.S. Transgender Survey, 78% of respondents reported wanting to receive gender-affirming hormone therapy at some point in their lives.3 Access to gender-affirming hormonal and surgical interventions is limited when HCPs are unprepared or unwilling to provide such services. In fact, transgender individuals have reported a lack of providers with expertise in transgender care as the largest barrier to accessing healthcare.4 Inadequate access to informed healthcare before, during, and after gender-affirming treatment may result in physical and emotional discomfort during examinations and neglect of routine reproductive and sexual healthcare.
Although mental health concerns in transgender and GNC individuals should not be automatically attributed to their gender identity, data do indicate higher rates of depression and suicidal ideation in these populations than in the general population.3,5,6 Fear of discrimination and actual discrimination are realities for transgender and GNC individuals in almost every aspect of their lives, causing chronic high levels of stress that can adversely affect mental health outcomes. To make matters worse, many transgender and GNC individuals may not feel comfortable seeking mental health care, fearing further discrimination.5
Indeed, barriers to accessing healthcare for transgender and GNC individuals go beyond the paucity of HCPs who are well prepared and willing to care for them. Many transgender and GNC individuals have faced implicit and explicit bias from both HCPs and office staff. In a recent national survey, one-third of transgender individuals who sought healthcare within the past year reported having an unpleasant experience with their HCP and nearly one-fourth reported not seeking healthcare when they needed it because of their fear of discrimination against them.2 HCP education must go beyond knowledge to address attitudes and behaviors necessary to provide a comfortable and safe healthcare environment that is normalized to persons of all gender identities. Adequate resources are important to support both HCPs and office staff in implementing respectful care that supports dignity and equality.
Implications for WHNP practice
Women’s health NPs (WHNPs) can play an important role in filling the need for HCPs who have the knowledge and cultural competence to provide reproductive and sexual healthcare for transgender and GNC individuals. As such, WHNPs should assess their current knowledge and experience related to providing care for transgender and GNC individuals and seek additional learning opportunities as needed. Table 2 provides a list of educational resources.
Reproductive and sexual health concerns for transgender and GNC individuals are in some respects similar to those of cisgender individuals and in other aspects unique. As with any patient, obtaining a comprehensive reproductive and sexual health history from your transgender and GNC patients is critical for tailoring and individualizing recommendations for screening, testing, and treatment. Recommendations for reproductive and sexual health screening are as follows:
- Cervical cancer screening for any individual with a cervix should be based on the same guidelines used for cisgender individuals.5,7
- Prostate cancer screening for any individual with a prostate should be based on the same guidelines used for cisgender individuals.1,5
- Sexually transmitted infection (STI) and HIV screening should be based on sexual behaviors and current anatomy.5,8
Recommendations regarding reproductive and sexual health counseling are as follows:
- Counseling regarding risk reduction for STIs and HIV should be based on sexual behaviors and current anatomy.
- Reproductive life planning should include discussion of the potential for becoming pregnant, the desire for pregnancy, and, as appropriate, discussion about contraceptive choices.
Reproductive and sexual health considerations unique to transgender individuals include the following:
Specific breast cancer screening recommendations for transgender women have not been established. However, the general consensus is that screening should not begin until after at least 5 years of estrogen use and then be performed within current age and risk factor recommendations for the general population.1,5
Transgender men who have not undergone chest reconstruction/mastectomy (including those who have had only breast reduction) should have breast cancer screening per current recommendations for cisgender women.1,5

Transgender men and GNC individuals may experience emotional and physical discomfort during pelvic examinations. Specific strategies should be used to maximize comfort and feelings of safety.1
- Information about gender-affirming hormone treatment, surgical procedures, and other interventions, as well as referral resources, should be readily available.
- Reproductive options and fertility preservation, if desired, should be discussed prior to initiation of gender-affirming medical or surgical treatment.
- It is within WHNPs’ scope of practice to provide gender-affirming hormone treatment using appropriate guidelines and resources (Table 3).1,5,9-11
Mental health considerations include the following:
- All patients, regardless of gender identity, should be screened for depression and suicidal ideation according to current guidelines.
- Mental health referrals should be provided, as needed, for transgender and GNC individuals to HCPs who are culturally competent to address these individuals’ specific needs.
Recommendations
NPWH recommends that WHNPs do the following:
- Engage in learning opportunities to enhance their ability to provide culturally competent, knowledgeable healthcare for transgender and GNC individuals.
- Provide a safe and trusted healthcare environment for transgender and GNC individuals, with implementation of inclusive nondiscrimination policies, use of gender-neutral language, written and verbal opportunities for patients to provide their chosen name and pronouns, and consistent use of these individuals’ chosen name and pronouns.
- Ensure that staff are appropriately trained and actively participate in all aspects of providing a safe and trusted healthcare environment for transgender and GNC patients.
- Provide reproductive and sexual health counseling, screening, testing, and examinations based on individual needs of patients, regardless of gender identity.
- Provide information about options for gender-affirming medical treatment and surgical procedures for patients who desire these services.
- Establish referral resources to ensure that patients have access to knowledgeable, culturally competent HCPs who can meet transgender and GNC individuals’ unique healthcare needs (if these needs cannot be fully met in one’s own clinical setting).
NPWH will provide leadership to ensure that:
- Continuing education programs are available for NPs to further their knowledge and cultural competency to meet the unique healthcare needs of transgender and GNC populations.
- NPs have resources available to guide the development and implementation of office policies related to nondiscrimination and inclusive healthcare environments.
- Educational programs for WHNP students include sexual and reproductive healthcare that is inclusive of transgender and GNC populations to prepare future NPs to provide evidence-based, culturally competent care for these individuals.
- Research regarding health disparities that affect transgender and GNC populations is encouraged and supported.
Approved by the NPWH Board of Directors: October 2017
References
Center of Excellence for Transgender Health, University of California San Francisco. Guidelines for the Primary and Gender-Affirming Care of Transgender and Gender Nonbinary People. 2016.
Lim FA, Brown DV Jr, Justin Kim SM. Addressing health care disparities in the lesbian, gay, bisexual, and transgender populations: a review of best practices. Am J Nurs. 2014;114(6):24-35.
James SE, Herman JL, Rankin S, et al. The Report of the 2015 U.S. Transgender Survey. Washington, DC: National Center for Transgender Equality; 2016.
Safer JD, Coleman E, Feldman J, et al. Barriers to health care for transgender individuals. Curr Opin Endocrinol Diabetes Obes. 2016;23(2):168-171.
Fenway Health. The Medical Care of Transgender Persons. 2015.
Nuttbrock L, Bockting W, Rosenblum A, et al. Gender abuse and major depression among transgender women: a prospective study of vulnerability and resilience. Am J Public Health. 2014;104(11):2191-2198.
American College of Obstetricians and Gynecologists. Committee Opinion No. 512. Health Care for Transgender Individuals. 2011.
CDC. Sexually Transmitted Diseases Treatment Guidelines, 2015.
Callen-Lorde Community Health Center, Transgender Health Services. Protocols for the Provision of Cross-Gender Hormone Therapy. 2012.
World Professional Association for Transgender Health. Standards of Care for the Health of Transsexual, Transgender, and Gender Nonconforming People. 7th Version. 2011.
Hembree WC, Cohen-Kettenis P, Delemarre-van de Waal HA, et al. Endocrine treatment of transsexual persons: An Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2009;94(9):3132-3154.

