The lockdowns and social isolation prompted by the COVID-19 pandemic in 2020 did not halt the rise in Sexually Transmitted Diseases (STDs), with congenital syphilis and gonorrhea continuing to increase, the Centers for Disease Control and Prevention said this week.
The lockdowns and social isolation prompted by the COVID-19 pandemic in 2020 did not halt the rise in Sexually Transmitted Diseases (STDs), with congenital syphilis and gonorrhea continuing to increase, the Centers for Disease Control and Prevention said this week.
“The COVID-19 pandemic increased awareness of a reality we’ve long known about STDs. Social and economic factors – such as poverty and health insurance status – create barriers, increase health risks, and often result in worse health outcomes for some people,” said Leandro Mena, MD, MPH, Director, CDC’s Division of STD Prevention. “If we are to make lasting progress against STDs in this country, we have to understand the systems that create inequities and work with partners to change them. No one can be left behind.”
In all, there were 2.4 million cases of STDs reported in 2020, the CDC said, despite a drop in cases in the beginning of the year, likely due to pandemic-related issues.
For example, chlamydia cases fell 13 percent in 2020, but the CDC notes that is likely because those infections are usually asymptomatic and identified through screening.
“Therefore, this decline is likely due to decreases in STD screening and underdiagnosis during the pandemic, rather than a reduction in new infections,” Mena wrote.
Still, chylamydia was the most common notifiable sexually transmitted infection in the country in 2020 at a rate of 481.3 cases per 100,000 population.
Gonorrhea is the second most common with 677,769 cases in 2020, an increase of 5.7%. Cases have more than doubled since 2009, CDC said.
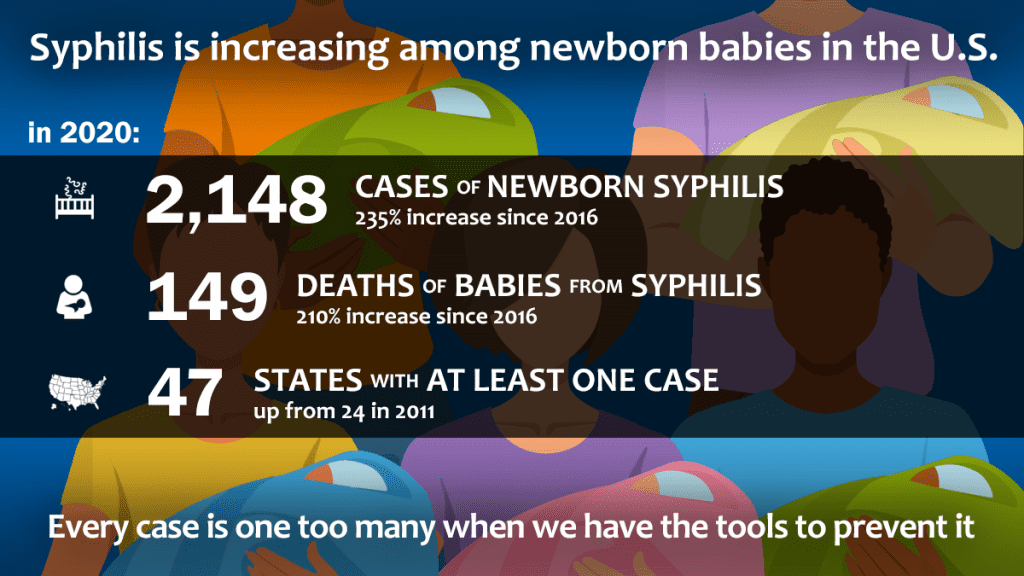
While a much smaller number, the rate of congenital syphilis has increased every year since 2013 and in 2020 there were 2,148 cases reported, which included 149 stillbirths and infant deaths. Those cases represent a 15% increase over the previous year and a more than 250% increase since 2016, mirroring an increase of primary and secondary syphilis among women ages 15-44.
The CDC notes that more than half of all STDs in 2020 were among adolescents and young adults age 15-24 and also disproportionately affect racial minority and Hispanic groups.
“Acknowledging inequities in STD rates is a critical first step toward empowering affected groups and the public health community to collaborate in addressing systemic inequities in the burden of disease — with the ultimate goal of minimizing the health impacts of STDs on individuals and populations,” the CDC observes.