By Nola Holness, PhD, CNM, APRN-Adult
One in five adolescent mothers in the United States has a repeat adolescent pregnancy, which is associated with increased maternal morbidity and mortality and poor birth outcomes. Whereas many adolescent mothers succumb to harmful external pressures, resulting in risky sexual behaviors and possible repeat pregnancy, others are fortunate in having a helpful support system. In addition, many adolescent mothers have an inner resilience and are able to implement measures on their own to prevent a repeat pregnancy. This study investigated how social influences and personal resilience affected African-American and Hispanic adolescent mothers’ planned use of contraception or abstinence to prevent a repeat adolescent pregnancy.
 Among developed countries in the world, the United States has the highest rate of adolescent pregnancy.1 Despite a recent decline in adolescent pregnancy rates in the U.S., one in five adolescent mothers has a repeat pregnancy.2 Once an adolescent gives birth to one infant, she has up to a 50% risk of having a second child within 12 months.3
Among developed countries in the world, the United States has the highest rate of adolescent pregnancy.1 Despite a recent decline in adolescent pregnancy rates in the U.S., one in five adolescent mothers has a repeat pregnancy.2 Once an adolescent gives birth to one infant, she has up to a 50% risk of having a second child within 12 months.3
Adolescent pregnancy, versus pregnancy at any other time during the reproductive years, carries the highest risks for maternal morbidity/mortality, low birth weight, and preterm birth.4,5 These risks increase with each subsequent pregnancy.4
Repeat adolescent pregnancies are also associated with escalating social and economic burdens that affect the adolescents, their families, their communities, and society at large, costing more than $9 billion annually.6 Adolescent mothers with more than one child are more likely to attain lower levels of education and live in poverty or remain on welfare.3
Large racial and ethnic disparities have persisted in adolescent pregnancy and birth rates over the years. In 2013, pregnancy rates among U.S. females aged 15-19 were 61/1,000 for Hispanics, 75/1,000 for non-Hispanic African Americans (AAs), and 30/1,000 for non-Hispanic whites.7,8 Also in 2013, birth rates among U.S. females aged 15-19 were 42/1,000 for Hispanics, 39/1,000 for non-Hispanic AAs, and 19/1,000 for non-Hispanic whites.7,8 In 2015, respective birth rates in these groups dropped to 35/1,000, 32/1,000, and 16/1,000.9 Also in 2015, the prevalence of repeat adolescent births in the U.S. was higher among Hispanics (18.7%) and non-Hispanic AAs (17.9%) than among non-Hispanic whites (14.3%).10
A study of adolescent mothers at high risk for a repeat pregnancy was conducted to ascertain the social ecological predictors of repeat adolescent pregnancy.11 Predictors included (1) planning to have another baby within 5 years, (2) failure to use long-acting contraceptives within 3 months of delivery, (3) not being in a relationship with the father of the first child 3 months post-delivery, (4) being more than 3 years younger than the first child’s father, (5) experiencing intimate partner violence within 3 months post-delivery, (6) not being in school 3 months post-delivery, and (7) having many friends who are adolescent parents.
Strategies to prevent repeat adolescent pregnancy
Contraceptive use
An increase in contraceptive use has contributed to a decrease in adolescent repeat pregnancy rates over the past two decades.12 Nevertheless, contraception use by minority adolescent mothers remains a challenge. In a review of more than 2,500 adolescent mothers, 45% of non-Hispanic whites used contraception, versus 23% of Hispanics and 21% of AAs.5 Barriers to continued contraceptive use by adolescent mothers include social environmental factors such as lack of parental support, lack of finances, and loss in continuity of care.13 Other barriers include having a partner who does not want to use contraception, having difficulty accessing contraceptives, and experiencing troublesome side effects related to contraceptives.14
Despite all these challenges, many adolescent mothers desire measures to prevent a repeat pregnancy, including use of more effective contraceptives.3 In 2012, the American College of Obstetricians and Gynecologists recommended that long-acting reversible contraceptives—the most effective contraceptives, which include intrauterine contraceptives (IUCs) and implants—be available for adolescent use.5,15 Adolescent mothers who were implant users, versus depot medroxyprogesterone acetate (DMPA) users and oral contraceptive users, were more likely to continue using their method.16 In addition, implant users were less likely to become pregnant than DMPA users or pill users.16 However, according to results of the Contraceptive CHOICE Project, the rate of IUC use among AA adolescent mothers remained lower, at 15%, than that among Hispanics (36%) or non-Hispanic whites (26.5%).17 Lack of knowledge about IUCs and cost of the devices are barriers to their use.18
Abstinence
Promotion of abstinence is another strategy to prevent repeat adolescent pregnancy. Although more than $200 million is spent on abstinence programs in the U.S. each year, a national analysis showed that the level of abstinence education—ranging from “no provision” to “covered” to “promoted” to “stressed”—was positively correlated with both adolescent pregnancy and adolescent birth rates.19 Abstinence-only education did not result in significant abstinence behavior; a more comprehensive approach is needed to reduce risky behaviors that can lead to adolescent pregnancy.19 Abstinence is a healthy behavioral option, but as a sole option for adolescents, it may be problematic.20
Effects of social influences and resilience in preventing repeat adolescent pregnancy
The occurrence or prevention of a repeat pregnancy in adolescent mothers may be related to social influences.8,21 Social influences are the effects of an interaction with another person or group on an individual’s thoughts, feelings, attitudes, or behaviors.22 For female adolescents, social influences may be exerted by parents, other family members, peers, or the father of their baby, any of whom may have either a beneficial or a detrimental effect on their risk for having a repeat pregnancy. Family dynamics (dysfunctional or supportive), identification with peers, school engagement, and spiritual orientation can also affect adolescents’ motivation to prevent a repeat pregnancy.
More than two-thirds of adolescent pregnancies are the result of sexual activity with a partner who is also an adolescent.23 Compared with their non-parenting peers, adolescent fathers tend to have less academic preparation, higher school dropout rates, and lower employment and income potential.23 Nevertheless, support from the father of their children can strengthen emotional bonds and enrich the home environment of adolescent mothers.24
Even under adverse circumstances, some adolescents are resilient enough to rebound from the effects of an unplanned pregnancy and even establish healthy behaviors to prevent a repeat adolescent pregnancy. Resilience is the ability to spring back in the face of adversity.25-27 In adolescents, resilience focuses on assets and resources that enable them to overcome the adverse effects of risk exposure.28
Assets and resources include personal qualities of intelligence, self-efficacy, self worth, hopefulness, and religious connection; having relatively higher socioeconomic status; attending good schools; and having other community advantages.29
As important as social influences and resilience are in their effect on adolescent mothers, few studies have specifically addressed these variables in the prevention of a repeat adolescent pregnancy. One study30 investigated pregnant Hispanics’ protective factors to prevent a repeat pregnancy, whereas another31 examined AA adolescents and their social and environmental stressors, without a focus on repeat pregnancies.
The study
Purpose
The aim of this study was to investigate the effects of social influences and resilience on intended contraceptive use or abstinence in terms of preventing a repeat adolescent pregnancy, specifically in AA and Hispanic parenting adolescent mothers. Research questions were as follows: (1) What is the relationship between social influences and personal resilience and the intention to use contraception or abstinence to prevent another pregnancy? and (2) What is the effect of the mother’s age, ethnicity, socioeconomic status, education, social influences, and resilience on her intention to use contraception or abstinence to prevent another pregnancy?
Methods
Study design
This study had a non-experimental, quantitative, cross-sectional design.
Sample
This convenience sample of adolescent mothers gave birth within 1-2 days of being recruited for the study at three hospitals within a tertiary hospital system in the Southeast U.S. Participants were recruited over a 6-month period. Letters of access were obtained from nursing directors of the women’s center at each hospital authorizing permission for access to its adolescent populations. Participants were recruited from the postpartum units of the hospitals by the principal investigator (PI). Inclusion criteria were AA or Hispanic female aged 10-19 years; delivery of a single, live, healthy, full-term infant; and being the major caretaker of the infant. Participants were also asked whether they were able to read English or Spanish on at least a fifth-grade level.
Data collection protocol
Data collection started once approval of the research protocol was secured from the University Office of Research Integrity and the collaborating hospital. First, the PI met with directors of nursing and staff at the three hospitals. The study and its importance were discussed at meetings to orient nurses and unit staff. Questions were answered. Subject recruitment posters were placed on postpartum units to encourage potential participants to volunteer for the study and as reminders for nurses and staff. Handouts were distributed at antepartum clinics to inform adolescents about the study to encourage their participation during the postpartum period.
The PI visited or called the postpartum units daily to identify potential participants and screen for eligibility. The study was explained and informed consent was obtained from adolescents aged 18 years or older. If prospective participants were younger than 18, the PI obtained informed consent from their parents or legal guardians, and assent was obtained from the adolescent mothers themselves. The study was conducted in each participant’s postpartum room. Participants were informed that the study packet could be completed in 50 minutes, although they could take as long as they needed to read and answer the questions. They were given the choice to complete the study packet in English or Spanish.
Adolescents were informed that participation in the study was voluntary; they could withdraw at any time, with no loss of service from the hospital or adverse repercussions from the university. No individually identifiable information was collected; each completed packet was stored in a sealed envelope, assigned a number, and transferred to a locked drawer in the PI’s office. As is the standard of care, several participants did initiate contraception prior to discharge from the hospital.
Instruments
The paper and pencil study packet consisted of a demographic data sheet; a list of contraceptive choices, including abstinence; the Adolescent Social Influence Scale (ASIS); and the Wagnild and Young Resilience Scale (RS).
Adolescent Social Influence Scale
The ASIS, an 11-point Likert-type questionnaire, is available in English and Spanish. The scale had been developed to compare and contrast social influences on Dominican adolescents living in the U.S. and those living in the Dominican Republic.32 Adolescents rated the influence of parents, family, peers, school, and church, ranging from 0 (no influence) to 10 (very strong influence). The reliability estimate was .78 with initial use of this instrument.32 Fathers of the babies were added as an additional social influence for this sample.
Wagnild and Young RS
Developed in 1993, this 25-item scale measures a person’s internal resources and how he/she copes with difficult life events.27 Items are constructed on a 7-point Likerttype scale from 1 (disagree) to 7 (agree). Based on the initial study using the scale, the reliability estimation was .91. Validity was supported with positive correlation with the Life Satisfaction Index A Scale and the Philadelphia Geriatric Center Morale Scale (r = .30 and r = .28, respectively; P <.001).The Spanish version of the scale had a Cronbach’s α of .93.33
Results
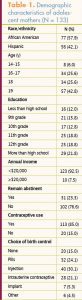 The sample comprised 133 participants, with 77 reporting their race/ethnicity as AA and 56 as Hispanic. Mean age was 17.8 years. To avoid another pregnancy, 85% of participants planned to use contraceptives and 23% planned to remain abstinent.
The sample comprised 133 participants, with 77 reporting their race/ethnicity as AA and 56 as Hispanic. Mean age was 17.8 years. To avoid another pregnancy, 85% of participants planned to use contraceptives and 23% planned to remain abstinent.
(Some participants planned to remain abstinent, yet wanted contraception on hand as needed.) The most common choices for intended birth control were DMPA injections and IUCs. Table 1 lists the demographic data collected.
1. What is the relationship between social influences and personal resilience and the intention to use contraception or abstinence to prevent another pregnancy?
African-American (mean [M], 36.9; standard deviation [SD], 12.82) and Hispanic (M, 34.2; SD, 14.66) mothers (t = .26), (P = .26) had similar social influences scores. The most significant social influences for the sample were parents (M, 8.2; SD, 2.97), followed by the father of the baby (M, 7.4; SD, 3.50). Parents had twice the degree of influence as friends (M, 4.1; SD, 3.46). Overall, school (M, 3.9; SD, 3.98) had the least influence. Reliability estimate for the ASIS was .72.
Resilience scores for AA adolescent mothers ranged from 57 to 175 (M, 145.8; SD, 21.59). Highest-scoring responses included the following: I usually manage one way or another, I am determined, I have self-discipline, and I have enough energy to do what I have to do. Hispanic adolescent mothers’ resilience scores were 65-174 (M, 142.8; SD, 20.70). Highest-scoring items were I can be on my own if I have to and I am friends with myself. Reliability estimates for the RS were .90 for the English version and .92 for the Spanish version.
Of all the point/bi-serial correlations, one significant positive correlation was found: AA adolescent mothers’ resilience and their intent to use contraception to prevent a repeat pregnancy (r = .366, P <.01) (Table 2). No correlation was found between social influences and intent to use contraception to prevent a repeat adolescent pregnancy.
2. What is the effect of the mother’s age, race, socioeconomic status, education, social influences, and resilience on using contraception to prevent a repeat adolescent pregnancy for AA and Hispanic parenting adolescent mothers?
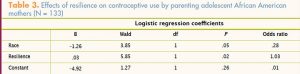
Logistic regression was used to analyze effects of the independent variables (age, race, socioeconomic status, education, social influences, and resilience) on the dependent variable of intending to use contraception to prevent a repeat pregnancy. The full model was statistically significant, x2 (11, N = 133) = 27.08, P =.004 (Table 3). Race and resilience were the two significant variables, with resilience (odds ratio [OR], 1.03) being the stronger predictor of adolescent mothers’ intent to use contraception as the method of preventing a repeat adolescent pregnancy. With other factors in the model controlled for, AA mothers were 3.6 times less likely than Hispanic mothers to use birth control (OR, .28) (Table 3).

Discussion
Major findings
Previous research has shown that resilient adolescent mothers have the ability to overcome barriers to contraceptive use in preventing an unintended repeat adolescent pregnancy.34,45 They can then rebound to achieve positive outcomes of finishing school, gaining employment, and becoming caring mothers.36 In the current study, resilient AA adolescent mothers reported that they were intent on using contraceptives, indicating that they possessed inner strengths and desires to prevent another adolescent pregnancy. At the same time, AA adolescent mothers, versus their Hispanic counterparts, were less likely to use contraceptives. Also in the current study, 23% of the participants indicated that they planned to remain abstinent as a birth control option. Resilient adolescent mothers, if equipped with cognitive and behavioral strategies and positive social influences, might be able to remain abstinent and therefore prevent a repeat pregnancy.37
Among social influences, parents were most important to both AA and Hispanic adolescent mothers in this study. Despite the important influence of peers,38 these adolescent mothers credited their parents with helping them strive to avoid another adolescent pregnancy. This finding is supported by the finding in two reports that parents, relative to friends, exerted a stronger influence on adolescents in terms of helping them avoid risky sexual practices and remain abstinent.39,40
Implications for practice
Although resilient AA adolescent mothers use contraception, they are less likely to use it than other adolescent mothers. Maternity healthcare personnel (e.g., obstetricians, midwives, nurse practitioners, nurses, social workers) are positioned to have a long-term impact on adolescent mothers through discussions about consistent contraceptive use, use of more effective birth control methods, and encouragement of abstinence and delay of sexual activity.14 It is recommended that sexually experienced adolescents who wish to become abstinent be supported in their decision.20
Parenting adolescents need the support of their own parents and family members. In addition, the father of the baby is an important social influence for the adolescent mother, as shown in this study. Maternity staff can facilitate the father’s involvement in the care of the adolescent mother and child in the immediate postpartum period and can engage him in dialogues on contraceptive use to prevent a repeat pregnancy.
Limitations
This study was conducted in a southern state in the U.S. and may lack generalizability. Participants were not asked if they were first-time or repeat adolescent mothers; gravidity and parity could explain some of the results.
Recommendations for future research
A longitudinal study with similar variables and varied time points over 2 years would reveal the impact of social influences and resilience on adolescent mothers’ contraceptive use or abstinence at a time when they are most likely to have a repeat adolescent pregnancy. Countries of origin among participants in this study included Chile, Colombia, Guatemala, Haiti, Honduras, Mexico, Nicaragua, and the United States. The cultural impact of one’s country of origin on decisions for contraceptive use or abstinence by minority adolescent mothers would be worthwhile to study.
Conclusion
Repeat adolescent pregnancy remains a national challenge. Among the most vulnerable groups, many AA adolescent mothers are underutilizing contraceptives, an effective method in preventing a repeat adolescent pregnancy. Resilient AA adolescent mothers are more likely to use birth control. Healthcare providers can initiate targeted conversations to promote the inner strength of vulnerable adolescent mothers to shun negative social influences that lead to risky sexual behaviors, rebound from an unplanned pregnancy, and avoid a repeat adolescent pregnancy.
Nola Holness is Clinical Assistant Professor at Florida International University in Miami, Florida. The author states that she has received financial support from the Florida Nurses Foundation (Undine Sam’s Award).
References
1. Sedgh G, Finer LB, Bankole A, et al. Adolescent pregnancy, birth, and abortion rates across countries:
levels and recent trends. J Adolesc Health. 2015;56(2):223-230.
2. CDC Vital Signs. Preventing Repeat Teen Births. April 2013.
3. Tocce KM, Sheeder JL, Teal SB. Rapid repeat pregnancy in adolescents: do immediate postpartum
contraceptive implants make a difference? Am J Obstet Gynecol. 2012;206(6):481.e1-7.
4. United Nations. The Millennium Development Goals Report. 2012.
5. Dee DL, Pazol K, Cox S, et al. Trends in repeat births and use of postpartum contraception
among teens-United States, 2004-2015. Morbid Mortal Wkly Rep. 2017:66(10):422-426.
6. Rosengard C. Confronting the intendedness of adolescent rapid repeat pregnancy. J Adolesc Health. 2009;44(1):5-6.
7. Guttmacher Institute. Pregnancies, Births and Abortions Among Adolescents and Young Women in the United States, 2013: National and State Trends by Age, Race and Ethnicity. September 2017.
8. Guttmacher Institute. Table 1.7.
9. CDC. National Vital Statistics Reports. Births: Final Data for 2015. January 5, 2017.
10. CDC. Trends in Repeat Births and Use of Postpartum Contraception Among Teens — United States, 2004–2015.
11. Raneri LG, Wiermann M. Social ecological predictors of repeat adolescent pregnancy. Perspect Sex Reprod Health. 2007;39(1):39-47.
12. Kost K, Henshaw S. Guttmacher Institute. U.S. Teenage Pregnancies, Births, and Abortions, 2010: National and State Trends by Age, Race and Ethnicity. May 2014.
13. Wilson EK, Samandari G, Koo HP, Tucker C. Adolescent mothers’ postpartum contraceptive use: a qualitative study. Perspect Sex Reprod Health. 2011;43(4):230-237.
14. CDC. Prepregnancy contraceptive use among teens with unintended pregnancies resulting in live births—Pregnancy Risk Assessment Monitoring System (PRAMS), 2004-2008. January 20, 2012.
15. Committee on Adolescent Health Care Long-Acting Reversible Contraception Working Group. The American College of Obstetricians and Gynecologists. Committee opinion no. 539: adolescents and long-acting reversible contraception: implants and intrauterine devices. Obstet Gynecol. 2012;120(4):983-988.
16. Lewis LN, Doherty DA, Hickey M, Skinner SR. Implanon as a contraceptive choice for teenage mothers: a comparison of contraceptive choices, acceptability, and repeat pregnancy. Contraception. 2010;81(5):421-426.
17. Peipert JF, Madden T, Allsworth JE, Secura GM. Preventing unintended pregnancies by providing no-cost contraception. Obstet Gynecol. 2012;120(6):1291-1297.
18. Fleming KL, Sokoloff A, Raine TR. Attitudes and beliefs about the intrauterine device among teenagers and young women. Contraception. 2010;82:178-182.
19. Stanger-Hall KF, Hall DW. Abstinence-only education and teen pregnancy rates: why we need comprehensive sex education in the U.S. PLoS ONE. 2011;6(10):e24658.
20. Santelli J, Ott MA, Lyon M, et al. Abstinence and abstinence-only education: a review of U.S. policies and programs. J Adolesc Health. 2006;38(1):72-81.
21. Patsdaughter CA, Kelley BR, Babington LM, Dyer JG. A comparison of sexual risk behaviors of Dominican adolescents in their homeland and in the United States. J Multicult Nurs Health. 2005;11(1):63-68.
22. Rashotte L. Social Influence. In: Ritzer G, Ryan JM. eds. The Concise Blackwell Encyclopedia of Sociology. Oxford, UK: Blackwell; 2009.
23. Klein JD; American Academy of Pediatrics Committee on Adolescence. Adolescent pregnancy: current trends and issues. Pediatrics. 2005;116(1):281-286.
24. Rozie-Battle J. Economic support and the dilemma of teen fathers. J Health Soc Pol. 2003;17(1):73-86.
25. Jacelon CS. The trait and process of resilience. J Adv Nurs. 1997;25(1):123-129.
26. Peterson SJ, Bredow TS. Middle Range Theories.2nd ed. Philadelphia, PA: Wolters Kluwer Health/ Lippincott Williams & Wilkins; 2009.
27. Wagnild G. A review of the Resilience Scale. J Nurs Meas. 2009;17(2):105-113.
28. Fergus S, Zimmerman MA. Adolescent resilience: a framework for understanding healthy development in the face of risk. Annu Rev Public Health. 2005;26:399-419.
29. Johnson JL, Wiechilt SA. Introduction to the special issue on resilience. Subst Use Misuse. 2004;39(5):657-670.
30. Cruz ME. Identifying individual, family, and education factors that protect Latina adolescents in alternative high schools from an early pregnancy. University of California, Santa Barbara, ProQuest Dissertations Publishing, 2011; 3495668.
31. House LE. And Still They Rise: An Examination of Risk and Protective Factors for Depression and Antisocial Behavior in African American Adolescents. Howard University, Pro-Quest Dissertations Publishing. 2001.
32. Babington LM, Kelley BR, Patsdaughter CA. Risk behaviors of Dominican adolescents in their homeland and in the United States. J Pediatr Health Care. 2007;21(6):372-380.
33. Heilemann MV, Lee K, Kury FS. Psychometric properties of the Spanish version of the Resilience Scale. J Nurs Meas. 2003;11(1):61-71.
34. Black C, Ford-Gilboe M. Adolescent mothers: resilience, family health work, and health-promoting practices. J Adv Nurs. 2004;48(4):351-360.
35. Romo LF, Segura DA Enhancing the resilience of young single mothers of color: a review of programs and services. JESPAR. 2010;15(1-2):173-185.
36. Porter L, Holness N. Breaking the repeat teen pregnancy cycle: how nurses can nurture resilience in at-risk teens. Nurs Womens Health. 2011;15(5):369-381.
37. Jemmott JB 3rd, Jemmott LS, Fong GT. Efficacy of a theory-based abstinence-only intervention over 24 months: a randomized controlled trial with young adolescents. Arch Pediatr Adolesc Med. 2010;164(2):152-159.
38. Harder A. The Developmental Stages of Erik Erikson. 2009.
39. Bouris A, Guilamo-Ramos V, Cherry K, et al. Preventing rapid repeat births among latina adolescents: the role of parents. Am J Public Health. 2012;102(10):1842-1847.
40. Cook EC, Buehler C, Henson R. Parents and peers as social influences to deter antisocial behaviors. J Youth Adolesc. 2009;38(9):1240-1252.

