The National Association of Nurse Practitioners in Women’s Health (NPWH) advocates for equitable access to informed, voluntary prepregnancy genetic carrier screening for individuals/couples who desire information about potential genetic reproductive risks. The goal of prepregnancy genetic carrier screening is to provide individuals/couples with information to assist them in understanding their reproductive risk for disease, family planning, considering reproductive options that align with their personal values and circumstances, and optimizing the opportunity to achieve a healthy pregnancy.1,2 Individuals/couples who are planning a pregnancy should be offered screening for the same genetic conditions as pregnant individuals/couples.3 To ensure informed choice regarding whether to pursue prepregnancy genetic carrier screening, healthcare providers (HCPs) must be knowledgeable, prepared, and willing to provide explanations of screening options including benefits and limitations within the context of the individual/couple’s personal and family health history and specific needs and values. Nurse practitioners (NPs) who provide care for individuals/couples who may be considering pregnancy have an important role in discussing prepregnancy carrier screening with them so that these individuals/couples can make informed decisions.
Policies should be in place in clinical settings as well as at local, state, and federal levels to protect the confidentiality of individuals and prevent discrimination regarding health, life, long-term care, and disability insurance based on screening test results. Genetic counseling should be available when any genetic condition carrier status is identified in one or both individuals of a reproductive couple so that all reproductive options can be discussed. Individuals must always have the autonomy to decline any or all screening, counseling, or follow-up testing.
NPWH supports ongoing research to advance knowledge in the area of genetic carrier screening. Research is also needed to increase understanding of what patients want and need to make informed decisions regarding screening and their level of satisfaction with all aspects of the screening and follow-up process.
Background
Carrier screening is a term used to describe genetic testing to determine if an individual who does not have an overt phenotype for a genetic disorder has a mutation or abnormal allele within a gene that is associated with a particular genetic disorder.1 Autosomal recessive diseases are genetic disorders that arise when both parents in a couple are carriers of the same recessive trait. When both individuals are carriers, the couple has a 1-in-4 risk of an affected child and a 1-in-2 risk of a child being a carrier with each pregnancy. Because carriers of recessive disorder traits are usually unaffected, children with recessive diseases are often born into families with no known history of the disease.4 Prepregnancy carrier screening allows individuals/couples to be informed about such reproductive risks. Professional guidelines recommend offering carrier screening for conditions that significantly affect quality of life as a result of cognitive or physical disability or need for lifelong medical therapies and in which the disability begins early in life.2
Carrier screening can be performed for one specific condition or for multiple disorders.1 Screening may be targeted, panethnic, or expanded. Targeted screening is often referred to as ethnic-specific screening and has long been the traditional approach. In this approach, screening decisions are based on disorders more frequently found in a specific ethnic or geographic population (eg, cystic fibrosis and Tay-Sachs disease in the Ashkenazi Jewish population, sickle-cell disease in African Americans). In addition, targeted screening may be based on the personal or family history behind a known or suspected autosomal or sex-linked recessive disorder.1
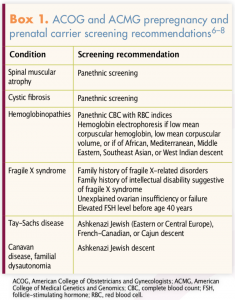 Panethnic screening, also referred to as nondirective screening, is an approach in which all individuals are offered testing for a specific set of disorders without regard to ethnicity or known familial risks. Rationales for the move to panethnic screening in the United States and other countries include the recognition of an increasing population of multiethnic individuals and that genetic conditions do not occur solely in specific ethnic groups.1,2,5 The American College of Obstetricians and Gynecologists (ACOG) and the American College of Medical Genetics and Genomics (ACMG) currently recommend panethnic screening be offered to all pregnant individuals and those considering pregnancy.6,7 Box 1 lists ACOG and ACMG screening recommendations for specific conditions.6–8 Box 2 provides links to more information from the National Institutes of Health Genetics Home Reference website about these conditions.9
Panethnic screening, also referred to as nondirective screening, is an approach in which all individuals are offered testing for a specific set of disorders without regard to ethnicity or known familial risks. Rationales for the move to panethnic screening in the United States and other countries include the recognition of an increasing population of multiethnic individuals and that genetic conditions do not occur solely in specific ethnic groups.1,2,5 The American College of Obstetricians and Gynecologists (ACOG) and the American College of Medical Genetics and Genomics (ACMG) currently recommend panethnic screening be offered to all pregnant individuals and those considering pregnancy.6,7 Box 1 lists ACOG and ACMG screening recommendations for specific conditions.6–8 Box 2 provides links to more information from the National Institutes of Health Genetics Home Reference website about these conditions.9
Expanded carrier screening refers to testing for several disorders at one time using a single sample. Expanded carrier screening panels are available that use next-generation sequencing methods with quick turnaround time and potentially lower costs.2,7 An advantage to the use of expanded carrier screening panels is the ability to identify individuals/couples at risk for carrying an affected child who could potentially be missed with current guideline-based targeted or panethnic screening.10,11 Expanded carrier screening panels in fact can provide individuals/couples with more information in making reproductive decisions. Of note, however, is the significant variability in the nature of conditions included and assay technologies used in these panels.10,12 Expanded carrier screening panels may include as few as 5 to 10 conditions or more than 100 disorders, including but not limited to autosomal recessive conditions.1,8
ACMG, ACOG, National Society of Genetic Counselors, Perinatal Quality Foundation, and Society for Maternal-Fetal Medicine published a joint statement in 2015 regarding points to consider in expanded carrier screening in reproductive medicine.2 ACOG has recommended consensus-determined criteria for condition inclusion in an expanded carrier screening panel. These criteria are carrier frequency of 1 in 100 or greater, well-defined phenotype, detrimental effect on quality of life, causing cognitive or physical impairment, requiring surgical or medical intervention, and having an onset early in life. Conditions primarily associated with an adult onset should not be included.1,5
Family history remains a crucial screening tool for prepregnancy assessment of the risk for inherited medical conditions and single-gene disorders.6,13 Opportunities for this screening include annual wellness visits as well as prepregnancy planning visits.13 When possible, the family history should include not only the patient but also the patient’s reproductive partner. Risk assessment should include known or suspected genetic conditions, ethnic background of family members, any known consanguinity, adverse pregnancy outcomes, cognitive or physical impairment of offspring, and newborn screening test results indicating an abnormality. Questionnaire and pedigree tools are available for this screening.13 Family risk assessment is used to stratify risks for genetic conditions and to aid in discussion of risks, benefits, and limitations of genetic carrier screening options. Of note, the use of expanded carrier screening panels does not replace the need for assessment of familial risks, recommended risk-based screening, or mandated newborn screening.1,2,5
HCPs may choose targeted, panethnic, and/or expanded carrier screening as acceptable strategies for use in their clinical practice.1 Whichever screening strategy or strategies is chosen, a consistent approach should be used in discussions with patients.2,14 The HCP should be able to provide clear, objective, and nondirective counseling so that the patient is well-informed about the benefits, limitations, and costs of tests in the context of specific needs and values.8,14 Discussion of limitations should include an explanation that screening will not identify all individuals at risk of the screened condition and that there is always some residual risk.1,7 If a patient requests carrier screening for a specific condition and such testing is readily available, the requested test should be offered after discussion of benefits and limitations regardless of ethnicity or family history.1,6
The patient should be informed of the protections and limitations of the Genetic Information Discrimination Act (GINA). GINA makes it illegal for health insurers to use genetic testing results to make decisions about coverage, rates, or preexisting conditions and for employers to discriminate against employees or applicants based on genetic information.14,15 GINA protection does not apply to long-term care insurance, disability insurance, or life insurance.14,15
When a patient is screened, results should be documented in the health record. If screening is negative for a specific condition or conditions, repeat testing at any time in the future is generally not warranted.5,6 If the patient is found to be a carrier for a specific condition, the individual’s reproductive partner should be offered testing for the same condition.6 If the patient and/or partner are carriers of a specific condition, genetic counseling should be offered. If a patient or partner is found to be a carrier for a specific condition, relatives are at risk of carrying the same mutation. Individuals should be encouraged to inform relatives of the risk and availability of carrier screening.6,14 The HCP should not disclose information without the permission of the patient.6,14
Individuals may choose to undergo prepregnancy genetic carrier screening for a variety of reasons regarding pregnancy planning.4,16 They may want information that helps them make decisions about the use of advanced reproductive technologies to decrease the risk of having a child with a specific disorder or so that they can plan for prenatal diagnostic testing. They may want to identify risks to learn more about the disorder, consider lifestyle changes they want to make if they have an affected child, and seek pediatric specialty providers and social support.6,16 Individuals also may choose not to have prepregnancy genetic carrier screening. They may decide positive results would be too anxiety producing, that pregnancy decisions would not change based on results, fear stigmatization or discrimination based on positive results, or that they do not want to incur the cost of screening.4,16 Regardless of an individual’s decision to undergo carrier screening or not, the opportunity to make an informed choice is important.6,16 Individuals who decide not to undergo prepregnancy carrier screening should be offered carrier screening during pregnancy with the same option to decline.
Recommendations
NPs who provide healthcare for reproductive-aged individuals/couples should:
• Engage in learning opportunities to expand their knowledge about prepregnancy genetic carrier screening, appropriate prescreening education for patients, and recommended follow-up when any genetic condition carrier status is identified in one or both individuals of a reproductive couple.
• Determine what screening strategy/strategies (targeted/ethnic, panethnic/nondirective, expanded) will be used in their healthcare setting.
• Establish policies within the healthcare setting that protect patient autonomy and confidentiality regarding carrier screening.
• Use patient education resources that are culturally and linguistically appropriate.
• Establish resources for genetic counseling for individuals and couples who are identified as genetic condition carriers.
NPWH will provide leadership and resources to ensure that:
• Continuing education programs are available for NPs to expand their knowledge about prepregnancy genetic carrier screening.
• NPs have informational materials for educating patients about prepregnancy genetic carrier screening.
• Research moves forward to advance knowledge in the area of genetic carrier screening, increase understanding of what patients want and need to make informed decisions, and evaluate patient satisfaction with all aspects of the screening and follow-up process.
• Policies regarding prepregnancy carrier screening support equitable access, protect patient autonomy and confidentiality, and prevent discrimination based on testing results.
References
- ACOG Committee on Genetics. Committee opinion no. 690: carrier screening in the age of genomic medicine. Obstet Gynecol. 2017;129(3):e35-e40.
- Edwards JG, Feldman G, Goldberg J, et al. Expanded carrier screening in reproductive medicine-points to consider: a joint statement of the American College of Medical Genetics and Genomics, American College of Obstetricians and Gynecologists, National Society of Genetic Counselors, Perinatal Quality Foundation, and Society for Maternal-Fetal Medicine. Obstet Gynecol. 2015;125(3):653-662.
- ACOG Committee on Gynecologic Practice. Committee opinion no. 762: prepregnancy counseling. Obstet Gynecol. 2019;133(1):e78-e89.
- Ong R, Howting D, Rea A, et al. Measuring the impact of genetic knowledge on intentions and attitudes of the community towards expanded preconception carrier screening. J Med Genet. 2018;55(11):744-752.
- Gregg AR, Edwards JG. Prenatal genetic carrier screening in the genomic age. Semin Perinatol. 2018;42(5):303-306.
- ACOG Committee on Genetics. Committee opinion no. 691: carrier screening for genetic conditions. Obstet Gynecol. 2017;129(3):e41-e55.
- Grody WW, Thompson BH, Gregg AR, et al. ACMG position statement on prenatal/preconception expanded carrier screening. Genet Med. 2013;15(6):482-483.
- Knutzen D, Stoll K. Beyond the brochure: innovations in clinical counseling practices for prenatal genetic testing options. J Perinat Neonatal Nurs. 2019;33(1):12-25.
- National Institutes of Health. Genetics home reference. Your guide to understanding genetic conditions. March 31, 2020. https://ghr.nlm.nih.gov/.
- Stevens B, Krstic N, Jones M, et al. Finding middle ground in constructing a clinically useful expanded carrier screening panel. Obstet Gynecol. 2017;130(2):279-284.
- Johansen Taber KA, Beauchamp KA, Lazarin GA, et al. Clinical utility of expanded carrier screening: results-guided actionability and outcomes. Genet Med. 2019;21(5):1041-1048.
- Beauchamp KA, Muzzey D, Wong KK, et al. Systematic design and comparison of expanded carrier screening panels. Genet Med. 2018;20(1):55-63.
- ACOG Committee on Genetics. Committee opinion no. 478: family history as a risk assessment tool. Obstet Gynecol. 2011;117(3):747-750.
- ACOG Committee on Genetics. Committee opinion no. 693: counseling about genetic testing and communication of genetic test results. Obstet Gynecol. 2017;129(4):e96-e101.
- ACOG. Patient resources. FAQs. Carrier screening. December 2018. https://www.acog.org/patient-resources/faqs/pregnancy/carrier-screening.
- Pereira N, Wood M, Luong E, et al. Expanded carrier screening in clinical practice: a current survey of patient impressions and attitudes. J Assist Reprod Genet. 2019;36(4):709-716.
Approved by NPWH Board of Directors: May 4, 2020

