As the Covid-19 pandemic progressed, it became apparent that the infection was more than just an acute illness for some but rather a prolonged syndrome. In the early days, some of those who were unable to fully recover termed themselves the “long haulers,” but now the collection of symptoms observed in these patients has come to be known as post-Covid conditions or long Covid.
The United States Census Bureau, in collaboration with other federal agencies, has collected data on the social and economic impacts of the pandemic on US households periodically since 2020 using what is called the Household Pulse Survey.1 Recent data from these ongoing surveys indicate that nearly 1 in 5 US adults have long Covid following a Covid-19 infection.1 Long Covid is almost twice as common in women as in men, especially among those age 50 to 59 years. Collected data also demonstrate that bisexual and transgender respondents reported higher rates of long Covid than those who reported other sexual orientations and gender identities.1 The highest rate of long Covid was reported in Hispanic adults followed by non-Hispanic White, Black, and Asian adults.1
Government recognition
In 2020, the World Health Organization recognized the post-Covid condition using the International Classification of Diseases, 10th revision (ICD-10) code of U09.3. This designation was later adopted by the US in 2021, making symptoms associated with the condition billable and reimbursable using ICD-10 code U09.9.2 The code should be for patients presenting with symptoms associated with a prior confirmed or presumed case of Covid-19 infection who no longer have acute symptoms.
Recognizing that these symptoms can be debilitating for some, long Covid became designated as a disability under the Americans with Disabilities Act and under the Affordable Care Act in 2021.3 This designation ensures that those persons significantly impacted by long Covid are protected from discrimination. Further information can be found at the Department of Justice website https://www.ada.gov/long_covid_joint_guidance.pdf and at the Health and Human Services website https://www.hhs.gov/civil-rights/for-providers/civil-rights-covid19/index.html.
In August 2022, the US Department of Health and Human Services created The National Research Action Plan to develop a better understanding of long Covid. The lengthy document outlines the government’s plan to accelerate and expand research and improve health equity while also focusing on improved patient care and outcomes. The plan intends to better define the full spectrum of symptoms of long Covid with continued focus on diagnostics, therapeutics, and interventions.4
In May 2023, the US Department of Health and Human Services declared an end to the Covid-19 public health emergency. Eventually the federal government will no longer purchase Covid-19 vaccines and treatments (eg, nirmatrelvir-ritonavir [Paxlovid]), likely impacting the payment for such services as well as coverage and access.5 In preparation for this change, the Department announced the “Bridge Access Program for Covid-19 Vaccines and Treatments” to maintain access to vaccines and treatments for the uninsured. Covid-19 vaccines are now recommended by the Advisory Committee on Immunization Practices as preventive healthcare, thus making access to these vaccines covered by most private insurers, Medicare Part B, Medicare Advantage plans, and Medicaid.5
Implications for providers
Although a positive antigen or NAAT [nucleic acid amplification test] for SARS-CoV-2 might aid in the diagnosis of long Covid, this is not required for making the diagnosis. Currently, there are no available laboratory studies for diagnosing long Covid, but instead the diagnosis is made from the patient’s presenting symptoms. Complicating the diagnosis is that symptoms can present differently from weeks to months or years and can be chronic or exhibit a relapsing-remitting pattern that can progress to life threatening. Long Covid is defined as not a single condition but rather many potentially overlapping entities that likely have different biologic causes and different risk factors and outcomes.4 Further confounding the diagnosis is that many of the more common symptoms associated with long Covid (fatigue, “brain fog,” depression, myalgias) also can be associated with myalgic encephalomyelitis/chronic fatigue syndrome, Lyme disease, and mast cell activation syndrome.2,6 The distinction is a new onset of symptoms associated with a prior history of Covid-19 infection. Symptoms of long Covid have been found to affect every body system, with more common symptoms including, but not limited to: fatigue and/or postexertional malaise (disabling and delayed exhaustion occurring hours or days later, disproportionate to the effort exerted and taking days or weeks to recover from); “brain fog” (impaired cognition and inability to concentrate); muscle pain; gastrointestinal symptoms to include nausea, loose stools, constipation, bloating, abdominal pain; cardiac symptoms such as tachycardia, chest pain, postural orthostatic tachycardia syndrome; depression; vision changes; insomnia and sleep changes; menstrual changes; erectile dysfunction; myalgias and arthralgias; cough; skin changes to include rashes; temperature intolerance; night sweats; peripheral vasoconstriction; and paresthesia.2,6,7
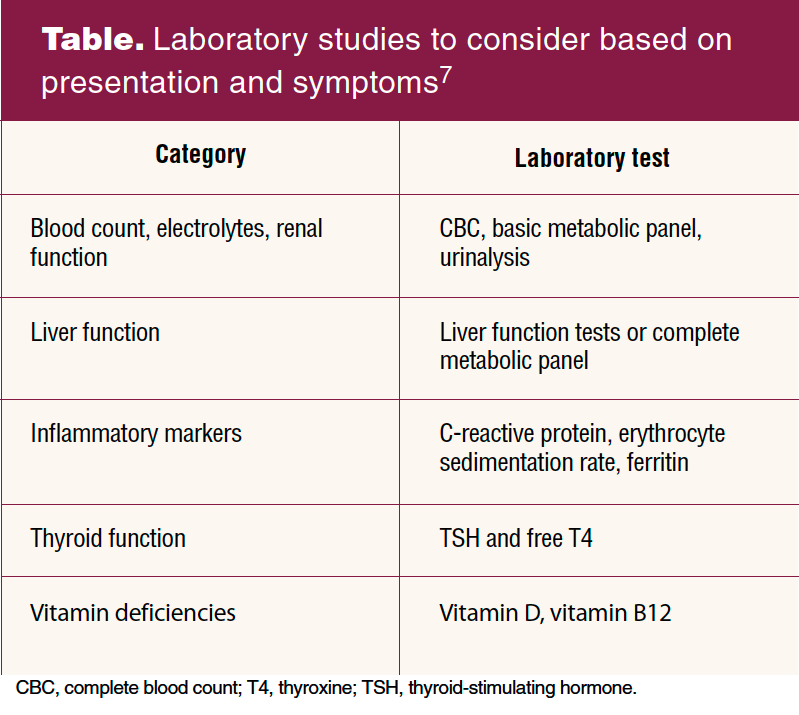
Based on patient history, physical examination, and clinical findings, laboratory studies and imaging may be necessary. However, normal findings on laboratory results and imaging do not negate the presence of long Covid or the impact these symptoms may be having on the patient’s daily functioning.7 Testing for non-Covid-19 related conditions that may be contributing to the illness but can be treated also may be indicated, especially if symptoms persist for 12 weeks or longer (Table).7
Most conditions associated with long Covid can be successfully managed by primary care providers with treatments that are specific to symptoms. Primary care providers can partner with specialists to improve outcomes with rehabilitation and for physical and mental wellbeing. Providers need to continuously monitor treatment throughout the course of the illness to recognize new symptoms and validate the patient’s concerns to optimize their quality of life. Ultimately, shared decision making and setting realistic treatment goals with patients will guide best practice and improve outcomes. Additional guidance and resources about long Covid for healthcare providers can be found at the Centers for Disease Control and Prevention.7
Erin Kiser is a nurse practitioner at the OB/Gyn Clinic, Womack Army Medical Center, in Fort Bragg, North Carolina. The author has no actual or potential conflicts of interest in relation to the contents of this article.
Womens Healthcare. 2023;11(4):46-48. doi: 10.51256/WHC082346
References
1 Centers for Disease Control and Prevention. National Center for Health Statistics. Nearly One in Five American Adults Who Have Had Covid-19 Still Have “Long Covid.” Data from the Household Pulse Survey. June 22, 2022. https://www.cdc.gov/nchs/pressroom/nchs_press_releases/2022/20220622.htm.
2 Bellanti JA. The long COVID syndrome: a conundrum for the allergist/immunologist. Allergy Asthma Proc. 2022;43(5):368-374.
3 United States Department of Justice. Office of Public Affairs. DOJ and HHS Issue Guidance on ‘Long COVID’ and Disability Rights Under the ADA, Section 504, and Section 1557. July 26, 2021. https://www.justice.gov/opa/pr/doj-and-hhs-issue-guidance-long-covid-and-disability-rights-under-ada-section-504-and-section.
4 US Department of Health and Human Services, Office of the Assistant Secretary for Health. National Research Action Plan on Long COVID. Washington, DC; August 2022.
5 US Department of Health and Human Services. Fact Sheet: End of the COVID-19 Public Health Emergency. May 9, 2023. https://www.hhs.gov/about/news/2023/05/09/fact-sheet-end-of-the-covid-19-public-health-emergency.html.
6 Herman E, Shih E, Cheng A. Long COVID: rapid evidence review. Am Fam Physician. 2022;106(5):523-532.
7 Centers for Disease Control and Prevention. Post-Covid Conditions: Information for Healthcare Providers. December 16, 2022. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/post-covid-conditions.html.