This article provides healthcare providers with up-to-date information about the impact of a variety of potentially toxic environmental exposures on reproductive health, specifically with respect to preconception care (PC) and interconception care (IC). PC/IC should include education regarding environmental risks and a discussion about ways to minimize a woman’s exposure to environmental toxins in order to optimize both pregnancy and infant outcomes.
A major focus of preconception care (PC) and interconception care (IC) is identification and mitigation/management of risk factors to improve health outcomes for women, newborns, and children.1 The importance of providing information about environmental toxins, as part of PC/IC to decrease risks of exposure, was recently highlighted by the International Federation of Gynecology and Obstetrics (FIGO).2 The American College of Obstetricians and Gynecologists (ACOG) includes information about environmental risks in its Good Health Before Pregnancy: Preconception Care patient guide.3 In this article, the authors describe what is known about some common environmental toxins and recommend strategies that healthcare providers (HCPs) can implement to help patients mitigate their risks of exposure.
Nearly all HCPs are aware of the dangers of smoking and drinking alcoholic beverages both prior to conception and during pregnancy, and counsel patients to avoid these practices. Also, before and after pregnancy is achieved, nearly all HCPs review patients’ medications to identify any potential teratogens and make adjustments as needed. Most HCPs advise pregnant patients to avoid eating fish high in mercury (e.g., shark, tilefish, swordfish, king mackerel).4 It also is common knowledge to recommend against consumption of soft cheeses and deli meats to decrease risk of exposure to listeria, and to remind patients to avoid exposure to toxins such as radiation, radon, and lead. Therefore, this article focuses on environmental risks about which HCPs may be less well informed.5
Environmental toxins are found in the air, in water, and in animals and plants that are consumed as food, as well as in products and furnishings in people’s homes. Adverse effects of exposure to high concentrations of such toxins in humans have been reported. It remains unclear, however, whether the lower concentrations of such toxins in the surrounding environment can potentially have the same adverse effects as do higher concentrations that are ingested or inhaled directly and on a regular basis.6
Endocrine disruptors
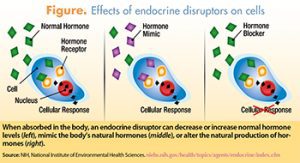
Many of these environmental toxins can act as endocrine disruptors; that is, they can interfere with endocrine system function at multiple levels and in multiple ways (Figure). During highly sensitive stages of human development, even small disturbances in endocrine function can have profound effects. With regard to the reproductive system and pregnancy outcomes, potential effects of endocrine disruption include fertility problems for both females and males, fetal growth restriction, physical malformations, neurologic/cognitive developmental disruptions, preterm birth, and increased future cancer risk.2,4,6-8 Many different categories of substances in the environment can serve as endocrine disruptors.
Pesticides/herbicides/fertilizers
Certain pesticides and herbicides may adversely affect fertility or they may have teratogenic effects if conception does occur. In addition, exposure to detectable amounts of pesticides has been linked to childhood leukemia and to neurologic and cardiovascular abnormalities in offspring.7 For example, exposure to organophosphate pesticides such as chlorpyrifos and diazinon has been associated with abnormal cognitive development in offspring.2,4,8
Consuming organically grown produce may limit one’s exposure to organophosphates used to control weeds and pests.7 Some non-organically grown produce is safer to consume than others. Readers are advised to check the Environmental Working Group’s (EWG’s) Shopper’s Guide to Pesticides in Produce, which has information on non-organic fruits and vegetables with low or high residues of organophosphates. Of note, residue from these organophosphates becomes embedded in the skin of the produce and/or penetrates into the produce and cannot be washed off.
Agricultural runoff from pesticides, herbicides, and fertilizers seeps into ground water. Exposure to the herbicide atrazine has been associated with reduced fetal growth.9 Nitrates in groundwater coming from fertilizers, manure, and human sewage have been associated with methemoglobinemia (blue baby syndrome) in infants and thyroid dysfunction in pregnant women.9 Although public water systems are tested for these contaminants and must meet safety standards, individuals who get drinking water from wells should be advised to have the water tested. Likewise, individuals whose drinking water comes from a public water system should ask for the latest test results for these substances.9 If test results are positive, home water filtration and/or reverse osmosis systems are recommended
Personal care products/cleaning products/paints
Many personal care products such as fragrances, cosmetics, soaps, lotions, and deodorants contain phthalates, which can act as endocrine disruptors.5,7 Phthalate exposure both prior to and during pregnancy has been linked to a risk for preterm birth and to neurodevelopmental and executive function problems in offspring.2,4 Males are more likely than females to be adversely affected by prenatal exposure to phthalates.4 In particular, male reproductive development abnormalities have been noted from in uteroexposure to these compounds.4,10 Best practice is to check the labels on personal care products and use only those that are phthalate free.
Triclosan, parabens, and triclocarbans, which are added to personal care products to provide antibacterial and antifungal effects, have been identified as endocrine disruptors that have been associated with preterm birth and low birth weight (LBW). In addition, exposure to triclosan may have thyrotoxic effects on the mother, which would have an adverse impact on the fetus.10 The EWG’s web page on Consumer Products is a good resource for information on high- and low-risk personal care and cleaning products.
Some organic compounds are not tightly chemically bound to the products containing them and can be released into the atmosphere in a process called off-gassing. Offgassed compounds can be inhaled directly from the atmosphere, but they also may settle on surfaces and be absorbed through the dermis by contact with such contaminated surfaces, or they may be ingested by hand-to-mouth transfer. This phenomenon is a concern when using latex-based paints and enamels. Exposure to these volatile organic compounds (VOCs) has been associated with increased allergy-related conditions in offspring such as rhinitis, asthma, and eczema.7 Use of low VOC-containing paints—recognizable by labels indicating this status—is recommended.
Housewares/furnishings/flame retardants
Many hard plastic containers contain bisphenol A (BPA), which acts as an endocrine disruptor and which has been associated with LBW in newborns and persistent wheezing, behavioral problems, and neurodevelopmental abnormalities, including problems with executive function, in offspring.2,4,7 Heating may increase release of BPA from these containers. Best practice is to not use these hard plastic containers or at least not use them to heat food in a microwave oven. Containers marked with a triangle containing the number 3 or the number 7 are made of soft plastics containing phthalates and pose the same risks as do personal care products containing phthalates.11
 Perfluorochemicals (PFCs) are used to make fluoropolymer coatings and products that resist heat, oil, stains, grease, and water. Fluoropolymer coatings can be used in products such as clothing, furniture, adhesives, food packaging, heat-resistant non-stick cooking surfaces, and the insulation of electrical wire. PFCs have been voluntarily eliminated from the market. However, because of their long half-lives, they persist in the environment and in wildlife and humans previously exposed to them. PFCs have been linked to thyroid problems and to adverse pregnancy outcomes related to prenatal exposure, although study results are inconsistent.9 As a health advisory, the Environmental Protection Agency has recommended that drinking water be evaluated for presence of perfluoroalkyl substances (PFASs), including PFCs such as perfluorooctanoic acid and perfluorooctanesulfonic acid.12 These PFASs can be removed from drinking water by carbon filtration and/or reverse osmosis.12
Perfluorochemicals (PFCs) are used to make fluoropolymer coatings and products that resist heat, oil, stains, grease, and water. Fluoropolymer coatings can be used in products such as clothing, furniture, adhesives, food packaging, heat-resistant non-stick cooking surfaces, and the insulation of electrical wire. PFCs have been voluntarily eliminated from the market. However, because of their long half-lives, they persist in the environment and in wildlife and humans previously exposed to them. PFCs have been linked to thyroid problems and to adverse pregnancy outcomes related to prenatal exposure, although study results are inconsistent.9 As a health advisory, the Environmental Protection Agency has recommended that drinking water be evaluated for presence of perfluoroalkyl substances (PFASs), including PFCs such as perfluorooctanoic acid and perfluorooctanesulfonic acid.12 These PFASs can be removed from drinking water by carbon filtration and/or reverse osmosis.12
Additive flame retardants such as polybrominated diphenyl ethers (PBDEs), widely used in furniture starting in the 1960s and 1970s, have been linked to endocrine disruption, impaired neurodevelopment, and increased risk for papillary thyroid cancer.2,7 Exposure to organophosphate flame retardants (PFRs), as quantified by urinary concentration of PFR metabolites in a study sample of 211 women, was shown to significantly impede the success of in vitro fertilization.13 Because of PBDEs’ long half-lives, any accumulation remains in the body for years.14
PBDEs were banned in Europe and voluntarily taken off the market in the United States in 2004. They were replaced by the flame retardant tris(1,3-dichloro-2 propyl)phosphate (TDCPP), which also disrupts endocrine function and has carcinogenic properties. TDCPP was voluntarily withdrawn from the market in 2015. However, both products—PBDE and TDCPP—were widely used in the foam of upholstered furniture, as well as in other foam cushion products (e.g., foam mattresses, pillows, bumper pads, automobile seats) and electronics. These chemicals are unstable in the foam and are released into the atmosphere via off-gassing, enabling them to be inhaled. In addition, these gases settle into household dust and create pathways for accumulation in the body through dermal absorption.
TDCPP is included in California Proposition 65’s list of carcinogenic products. Good hand washing can decrease exposure to this compound.14,15 Another recommended practice is to check the tag on upholstered furniture to determine whether it meets California TB117 fire safety standards and then avoidsuch furniture to limit exposure to these flame retardants.16,17 Finally, if possible, polyurethane foam should be avoided in favor of products that use polyester fiber filling for cushioning. Polyester fiber fillings are not treated with flame-retardant chemicals.
Polycyclic aromatic hydrocarbons and particulate matter
Living near a highway, which increases one’s exposure to polycyclic aromatic hydrocarbons (byproducts of fuel burning) and high levels of particulate matter (PM), is associated with increased risk for preterm labor and the development of autism spectrum disorder (ASD) and other cognitive problems in offspring.4,7,18
Preterm labor and ASD have also been associated with spending a lot of time driving in internal combustion engine-powered vehicles, with resultant higher exposure to exhaust containing benzene and other volatile gases such as polycyclic aromatic hydrocarbons.4,7,18 Traffic-related exposure to nitrogen dioxide and to PM <2.5 micrometers in diameter (PM2.5) and <10 micrometers in diameter (PM10) is also associated with ASD development.18 The risk related to long commutes or an occupation involving driving an internal combustion engine-powered vehicle can be mitigated by having a good filtration system in the vehicle.7
Exposure to ozone and fine PM (PM2.5 and PM10) in the air also is associated with preterm delivery and risk for pregnancy-related hypertension. 7 Therefore, paying attention to low-quality air alerts and staying indoors in a setting with a good filtration system for cooling and heating systems is a prudent practice for every woman of childbearing age, not just those with chronic respiratory conditions.
Solvents
In its Good Health Before Pregnancy: Preconception Care patient guide, ACOG advises women to check with their employers about potential exposure to solvents.3 Prenatal exposure to solvents such as toluene has long been known to be harmful to offspring. Exposure to chlorinated solvents has been associated with increased risk for ASD.18 Presence in drinking water of a product used in dry cleaning, tetrachoroethylene (perchlorethylene or PERC), has been linked to neurologic problems and the development of neurodegenerative disorders such as Parkinson’s disease later in life.4 Although many dry cleaners are replacing PERC with safer chemicals, long-term exposure remains a concern and is associated with adverse pregnancy outcomes.7,19
Potential emerging environmental risks
Concern exists regarding the possibility that banned substances such as polychlorinated biphenyls (PCBs), which have been associated with adverse neurodevelopmental effects, may increase again in the environment.9 The return of PCBs is related to melting of the polar ice caps in which they may be trapped. Information is also emerging about possible harms from electromagnetic radiation exposures, nanoparticles, and genetically modified organisms.7 These risks need further study before inclusion in PC/IC recommendations.
Resources and recommendations
Preconception care and interconception care should include the provision to patients of evidence-based information on potential environmental toxins and how to reduce risks of exposure. In today’s often time-limited visits, HCPs may have difficulty covering everything important in PC/IC. Written materials such as ACOG’s Good Health Before Pregnancy: Preconception Care and websites such as those listed in the Box can be helpful.
Healthcare providers are encouraged by FIGO to engage in advocacy to decrease the widespread use of identified environmental toxins.2 In 2015, scientists, health professionals, and children’s health advocates joined together in Project TENDR: Targeting Environmental Neuro-Developmental Risks. Project TENDR developed a consensus statement supporting assessment, monitoring, and reduction of exposures to environmental toxins in order to promote health for children in the U.S.20 The seriousness of the risks to the current generation and the potential intergenerational risks related to possible epigenetic changes associated with toxic environmental exposures make providing information to patients about these risks imperative.
Diane Schadewald is Clinical Associate Professor at the University of Wisconsin-Milwaukee College of Nursing. Ursula A. Pritham is Associate Professor at Georgia Southern University School of Nursing in Statesboro. The authors state that they do not have a financial interest in or other relationship with any commercial product named in this article.
References
- Rosener SE, Barr WB, Frayne DJ, et al. Interconception care for mothers during well-child visits with family physicians: An IMPLICIT Network Study. Ann Fam Med. 2016;14(4):350-355.
- Di Renzo GC, Conry JA, Blake J. et al. International Federation of Gynecology and Obstetrics opinion on reproductive health impacts of exposure to toxic environmental chemicals. Int J Gynaecol Obstet. 2015;131(3):219-225.
- American College of Obstetricians and Gynecologists. Good Health Before Pregnancy: Preconception Care. FAQ056. 2015.
- Grandjean P, Landrigan PJ. Neurobehavioural effect of developmental toxicity. Lancet Neurol. 2014;13(3):330-338.
- Chan LM, Chalupka SM, Barrett R. Female college student awareness of exposures to environmental toxins in personal care products and their effect on preconceptual health. Workplace Health Saf.2015;63(2):64-70.
- U.S. Environmental Protection Agency. Endocrine Disruption. Last updated on February 22, 2017.
- Genuis SJ, Genuis RA. Preconception care: a new standard of care within Maternal Health Services. Biomed Res Int. 2016;2016:6150976.
- Engel SM, Wetmur J, Chen J, et al. Prenatal exposure to organophosphates, paraoxonase 1, and cognitive development in childhood. Environ Health Perspect. 2011;119(8):1182-1188.
- America’s Children and the Environment, Third Edition. Washington, DC: U.S. Environmental Protection Agency; 2013.
- Geer LA, Pycke BF, Waxenbaum J, et al. Association of birth outcomes with fetal exposure to parabens, triclosan, and triclocarban in an immigrant population in Brooklyn, New York. J Hazard Mater. 2017;323(Pt A):177-183.
- Sathyanarayana S, Forcareta J, Dailey T, Buchanan S. Environmental exposures: how to counsel preconception and prenatal patients in the clinical setting. Am J Obstet Gynecol. 2012;207(6):463-470.
- U.S. Environmental Protection Agency. Fact Sheet: PFOA & PFOS Drinking Water Health Advisories. November 2016.
- Carignan CC, Mínguez-Alarcón, L, Butt, CM, et al. Urinary concentrations of organophosphate flame retardant metabolites and pregnancy outcomes among women undergoing in vitro fertilization. Environ Health Perspect. 2017;125(8):087018.
- Betts KS. Exposure to TDCPP appears to be widespread. Environ Health Perspect. 2013;121(5):A150.
- Carignan CC, McClean MD, Cooper EM, et al. Predictors of tris(1,3-dichloro- 2-propyl) phosphate metabolite in the urine of office workers. Environ Int. 2013;55:56-61.
- Stapleton HM, Sharma S, Getzinger G, et al. Novel and high volume use of flame retardants in US couches reflective of the 2005 PentaBDE phase out. Environ Sci Technol. 2012;46(24):13432-13439.
- Cooper EM, Kroeger G, Davis K, et al. Results from screening polyurethane foam based consumer products for flame retardant chemicals: assessing impact on the change in the furniture flammability standards. Environ Sci Technol. 2016;50(19):10653-10660.
- Lyall K, Schmidt RJ, Hertz-Picciotto I. Maternal lifestyle and environmental risk factors for autism spectrum disorders. Int J Epidemiol.2014;43(2):443-464.
- Lucas D, Hervé A, Lucas R, et al. Assessment of exposure to perchloroethylene and its clinical repercussions for 50 dry-cleaning employees.J Occup Environ Hyg. 2015;12(11):767-773.
- Bennett D, Bellinger DC, Birnbaum LS, et al. Project TENDR: Targeting Environmental Neuro-Developmental Risks. The TENDR Consensus Statement. Environ Health Perspect.2016;124(7):A118-A122

