By Helen A. Carcio, MS, MEd, ANP-BC
Clinical evaluation of the pelvic floor muscles (PFMs) should be an integral part of a comprehensive well-woman examination because it can aid in identifying bladder dysfunction and pelvic organ prolapse. Digital assessment of the PFMs, a simple but neglected technique that should be part of every clinical evaluation of the pelvic musculature, is described in detail in this article.
As female Baby Boomers age, they are likely to experience pelvic health problems with increasing frequency.1 Knowledge of the female pelvic musculature is essential to understanding the pathophysiology of conditions such as urinary incontinence (UI) and pelvic organ prolapse (POP). In addition, this knowledge helps examiners more accurately interpret findings from a digital pelvic examination. Conditions such as UI usually occur as result of a dysfunction of the bladder and/or the urethra along with, in most cases, weakness of the pelvic floor muscles (PFMs).2
The pelvic floor explained
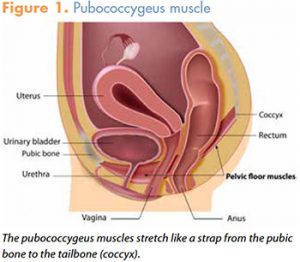
The pelvic floor, also called the pelvic diaphragm, is a bowl-shaped muscular sheet whose main functions are to support the abdominal and pelvic organs and to control the opening and closing of the urethral and anal sphinters.3 The pelvic floor rests at the bottom of the pelvis and is formed mainly by the levator ani muscle group. The pubococcygeus muscle forms the anterior portion of the levator ani and is responsible primarily for maintaining continence. The pubococcygeus (PC), as the name implies, stretches like a muscular trampoline from the pubic bone, where it arises, to the coccyx, where it inserts (Figure 1). Three holes (the levator hiatus) open into and through this muscular band. In women, these structures are the urethra, the vagina, and the anal canal, the first of which regulates the flow of liquid waste and the lattermost of which regulates the flow of solid waste as these materials pass out of the body.
When intact, the pelvic floor forms a tight occlusive layer on which the pelvic organs rest, preventing these organs from falling through the opening between the pelvic bones and stabilizing and protecting them during periods of increased intra-abdominal pressure such as that which occurs during childbirth. In addition, the pelvic floor controls and tightens the sphincters around the urethra and the anal canal to maintain continence.
The PFMs work differently from most other muscles in the body, which are usually in a state of relaxation unless performing a task. By contrast, the PFMs continuously maintain a low level of contraction, which allows them to continuously stabilize and support the pelvic organs. When the PFMs are actively contracted, the bladder is elevated further up in the pelvis, the bladder neck is stabilized, and, most important, the angle of the bladder neck remains partially bent, much like a flexible straw, to obstruct the flow of urine from the bladder. If the PFMs weaken (risk factors for PFM weakness are listed in Table 1), the bladder drops lower in the pelvis and the bladder neck angle straightens, resulting in a freer flow of urine—and UI.4

Urinary continence requires an intact, intrinsic urethral sphincter; a well-supported bladder neck and urethra; and intact PFMs.5 When a woman contracts her PFMs, she is actually tightening and lifting the levator ani muscle group, which contracts (pulls) against the PC muscle—the same muscle that is strengthened with Kegel exercises.
Clinical evaluation
A short series of questions and a digital pelvic examination are all that are needed to diagnose most pelvic health problems and initiate a well-structured, conservative treatment plan.
Health history
The health history begins by asking the patient a simple question: Have you leaked urine in the past 3 months? If she responds yes, then the nurse practitioner (NP) asks whether the leakage is associated with impact such as jogging or coughing (stress UI) or whether it is accompanied by a strong feeling of urgency, even leaking, when the patient approaches the bathroom (urge UI/overactive bladder). The Minute Quiz for Urinary Incontinence, a short questionnaire created by the author, may also be used (Table 2).

Inspection
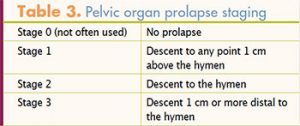
The patient assumes a comfortable semi-Fowler’s position for this examination. The NP spreads the patient’s labia and observes for any gaping of the introitus or visible descent of pelvic structures as the patient bears down or coughs. In addition, the NP looks for any concomitant bulging of the bladder or rectum or leaking of urine. Next, the NP records the stage of descent of any POP (Table 3). If a prolapse is suspected, the patient is asked to stand, which allows visualization of the full extent of it.6 She may place her hands on the NP’s shoulders for stability or elevate one leg on a stool to provide better visualization of the vulva. The NP palpates the vaginal opening for any bulges as the patient bears down again.
Digital assessment of the pelvic floor muscles
Evaluation of PFM strength provides a quantitative assessment of the voluntary contraction of these muscles. Digital assessment is essential to evaluating PFM strength and also enables the NP to detect the presence of a prolapse, a mass, or weakened PFMs or the presence of any conditions related to the aforementioned risk factors that could progress to PFM dysfunction.
Teaching the rectal squeeze
The patient resumes her position on the exam table. The NP asks her to relax her abdominal muscles and then tighten her rectal muscles when directed to do so. The NP explains that PFM tightening—the Kegel exercise—actually entails performing a rectal muscle squeeze. This exercise can be accomplished by pretending to prevent oneself from passing gas.7 As the PFMs are tightened rectally, they pull against the pubic bone anteriorly and lift and tighten the PC muscle. Of note, many women think, or they are taught—erroneously so—that the Kegel exercise involves performing a vaginal squeeze or pretending to stop the flow of urine. These latter practices are counterproductive to PFM strengthening.
The NP should observe the anus as the patient squeezes her rectal sphincter. The introitus and anal sphincter should pucker and draw in. Again, the NP should reinforce that the Kegel exercise, or PFM strengthening, is always a rectal squeeze. Of note, many women will have difficulty switching from a vaginal squeeze to a rectal squeeze if the former is already a regular practice.
Assessment of pelvic tightening
Assessment of the patient’s ability to tighten the PFMs and relax the abdomen is vital to the correct diagnosis of bladder dysfunction or POP. The NP begins this part of the exam by inserting one or two fingers about 3-6 cm (first knuckle) inside the vagina, at the 5 and 7 o’clock positions around the external vaginal opening. While the patient squeezes the PC muscle, the NP palpates both of its branches and notes her ability to sustain the squeeze. During the squeeze, the muscle should feel like a tight band. The contraction draws the rectum and vagina upward and forward, toward the symphysis pubis, in an attempt to tighten and close the vagina. If the patient is asked to perform multiple squeezes, she should relax the muscle completely between squeezes.
The NP grades the strength of the squeeze, its duration, and whether any deflection of the fingers is felt (Table 4). A low score indicates a lack of PFM strength. The higher the score, the more effectively the patient is performing the Kegel exercise; she should strive for a level 3 in all parameters. The NP can also use this scale as a means of positive reinforcement; the patient can track her increasing PFM strength at each subsequent visit.
![]()
Promotion of abdominal relaxation
As the woman tightens her PC muscle, she must concomitantly relax her abdominal muscles. (Simultaneous contraction of the abdominal muscles reduces the strength of the rectal tightening she can perform.) The NP places the opposite hand lightly on the patient’s abdominal muscles to monitor for any incorrect straining. The abdomen should remain soft. This type of biofeedback gives welcome reassurance to the patient that she is performing the exercises correctly.
In addition to relaxing her abdominal muscles and isolating/contracting the PFMs, the patient must relax her accessory muscles, which she may unknowingly be squeezing in an attempt to recruit other muscles to help her tighten her vagina. Tightening would almost entirely negate the usefulness of performing the Kegel exercise. To promote relaxation of the accessory muscles, which include those of the abdomen, thighs, and buttocks, the NP can tell her: No abs, hips, or butts! NPs may also need to remind the patient to avoid pushing against the stirrups to enhance her vaginal squeezing ability. This effort is also counterproductive.
Teaching correct performance of PFM exercises
Once the digital assessment of the PFMs is complete, the NP can teach the patient how to perform PFM strengthening exercises. Figure 2 provides full instructions. The patient should tighten and relax her PFMs 10 times in a row at least 3 times a day. Performing PFM exercises can significantly reduce the incidence of conditions associated with PFM weakness.8

A reimbursable event
If PFM weakness is present, the NP can attach the billable ICD-10 procedural codes N81.84 (disuse atrophy of pelvic muscle and anal sphincter) and N81.9 (female genital prolapse).
Conclusion
Once the NP becomes comfortable with them, these questions and maneuvers should take only a few extra minutes in the exam room. Digital assessment, a simple but sometimes neglected technique, should be added to every pelvic examination, even if a patient does not have any UI or POP concerns. This simple assessment could change the face of continence care for generations to come as women, particularly younger women, are taught how to increase PFM awareness and maintain and tone their PFMs via Kegel exercises, which can prevent pelvic health problems in the future.
Helen A. Carcio is Director of the Health & Continence Institute for Health Professionals. She travels nationally, teaching other NPs how to establish pelvic health centers, which provide a much-needed clinical service for aging female Baby Boomers. Readers can reach the author at hcarcio@aol.com. The author states that she does not have a financial interest in or other relationship with any commercial product named in this article.
References
- Gibbs CF, Johnson TM 2nd, Ouslander JG. Office management of geriatric urinary incontinence. Am J Med. 2007;120(3):211-220.
- Rogers RG. Clinical practice. Urinary stress incontinence in women. N Engl J Med. 2008;358(10):1029-1036.
- Bharucha AE. Pelvic floor: anatomy and function. Neurogastroenterol Motil. 2006;18(7):507-519.
- Ashton-Miller JA, Howard D, DeLancey JO. The functional anatomy of the female pelvic floor and stress continence control system. Scand J Urol Nephrol Suppl. 2001;207:1-7.
- DeLancey JO. Structural support of the urethra as it relates to stress urinary incontinence: the hammock hypothesis. Am J Obstet Gynecol. 1994;170(6):1713-1720.
- Delancey JO. Anatomy and biomechanics of genital prolapse. Clin Obstet Gynecol. 1993;36(4):897-909.
- Kegel AH. Progressive resistance exercise in the functional restoration of the perineal muscles. Am J Obstet Gynecol. 1948;56:238-249.
- Bo K. Pelvic floor muscle training is effective in treatment of female stress urinary incontinence, but how does it work? Int Urogynecol J Pelvic Floor Dysfunct. 2004;15(2):76-84.

