Brooke M. Faught
Bacterial vaginosis (BV) is the most prevalent vaginal infection. Although BV is not classified as a sexually transmitted infection, it is considered a sexually associated infection. As such, it may be possible to reduce the chance of developing it or at least reduce the rate of recurrences. Both acute and recurrent BV can have a direct impact on a woman’s perceptions about her body and her sexual health, which can then have an adverse effect on her sexual activities and quality of life. What can healthcare providers do to help?
Bacterial vaginosis (BV) is a polymicrobrial condition that occurs when the normal vaginal flora shifts to include an overabundance of anaerobic bacteria such as Gardnerella vaginalis, Escherichia coli, and Atopobium vaginae.1,2 Common symptoms of BV, the most prevalent symptomatic vaginal condition, include vaginal odor and discharge; less common are vulvovaginal itching and burning.2-4 Although these symptoms are more annoying than directly harmful, BV can be associated with serious co-morbidities such as sexually transmitted infections (STIs), pelvic inflammatory disease (PID), pregnancy loss, preterm birth, and postpartum and post-abortion endometritis.4-7
BV, sexual activity, and STIs
Overall BV prevalence in the United States is 29% among women aged 14-49 years, making it the most common vaginal infection in this age group.8-10 BV prevalence in women who have sex with women (WSW) is 25%-50%.11,12 The higher rates of BV reported in WSW are associated with receptive oral sex, a higher lifetime number of female partners, failure to clean previously used insertive sex toys before use, and anilingus with a female partner.11,13
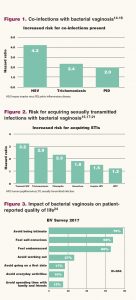
Compared with women who do not have BV, those with BV are more likely to have co-existing herpes simplex virus infection, trichomoniasis, and PID (Figure 1).14-16 Women with BV but no co-existing infections, when compared with women without BV, are more likely to contract trichomoniasis, chlamydia, gonorrhea, and human papillomavirus infection (Figure 2).15,17-21 In addition, women with BV are more susceptible to contracting HIV infection, and HIV-positive women have a higher incidence of BV.17 Furthermore, women with BV/HIV have an increased risk for female-to-male HIV-1 transmission and those with BV-associated bacterium 1, 2, or 3 and HIV have an increased viral shedding of HIV-1.17,22
BV and sexual health quality of life
Bacterial vaginosis can have a major adverse impact on women’s quality of life (QOL), including their sexual health QOL. Almost all women with BV report feeling self-conscious, embarrassed, and uncomfortable in social situations because of their symptoms.1,23,24 Many women with BV attribute their symptoms to sexual activity.25 In a survey of 304 women, nearly 80% of respondents reported avoiding sexual activity because of BV symptoms.24 In addition, women with BV reported avoidance of working out, going on first dates, performing everyday activities, and spending time with family and friends (Figure 3).24
The healthcare provider role in prevention, treatment, and patient education
Some women excessively cleanse their vulvovaginal area in the mistaken belief that BV is related to poor hygiene and that cleansing themselves in this way can help prevent the condition.23 Women need to understand that the healthy vagina self-maintains a balanced ecosystem, including the presence of lactobacilli species,26,27 and that excessive cleansing is unnecessary. In fact, they should wash the vulva with warm water only. Many over-the-counter (OTC) products marketed for feminine health may actually increase a woman’s risk for developing BV by causing a shift in the normal vaginal pH and disrupting the growth of protective lactobacilli species.27
Published data remain inconsistent on the impact of semen on the vaginal ecosystem, although some evidence suggests an association between semen exposure and BV.30 For women with a history of BV or ongoing BV who want to remain sexually active, HCPs should advise them to practice consistent condom usage with their partners and to be sure to wash sexual aids and toys before and after each use. Evidence also suggests avoidance of anilingus may reduce the incidence of BV.11,13
Conclusion
Bacterial vaginosis is more than just a nuisance condition. Women are at an increased risk for acquiring STIs, more likely to transmit HIV, and have a higher potential for pregnancy loss and preterm birth. Women with BV can experience substantial diminution of their self-esteem and a decline in their sexual health QOL as a result of the condition, especially if they have recurrent BV. HCPs must educate women about how to reduce their chance of developing BV, recognize the symptoms of BV, follow the treatment regimen prescribed for them, and understand best practices to prevent BV recurrences.
Brooke M. Faught is a women’s health nurse practitioner and the Director of the Women’s Institute for Sexual Health (WISH), a division of Urology Associates, in Nashville, Tennessee. She is a Fellow of the International Society for the Study of Women’s Sexual Health (ISSWSH) and a NAMS certified menopause practitioner. The author states that she serves as a speaker and an advisory board member for AMAG, Duchesnay, Lupin, and Therapeutics MD and as an advisory board member for Trophikos.
References
- Bilardi JE, Walker S, Temple-Smith M, et al. The burden of bacterial vaginosis: women’s experience of the physical, emotional, sexual and social impact of living with recurrent bacterial vaginosis. PloS One. 2013;8(9):e74378.
- Workowski KA, Bolan GA; CDC. Sexually transmitted diseases treatment guidelines, 2015. MMWR Recomm Rep. 2015;64(RR-03):1-137.
- ACOG Committee on Practice Bulletins—Gynecology. ACOG Practice Bulletin. Clinical management guidelines for obstetrician-gynecologists, Number 72, May 2006: Vaginitis. Obstet Gynecol. 2006;107(5):1195-1206.
- Sobel JD. Editorial Commentary: Vaginal Biofilm: Much Ado about Nothing, or a New Therapeutic Challenge? Clin Infect Dis. 2015;61(4):607-608.
- van Oostrum N, De Sutter P, Meys J, Verstraelen H. Risks associated with bacterial vaginosis in infertility patients: a systematic review and meta-analysis. Hum Reprod. 2000;28(7):1809-1815.
- Nelson TM, Borgogna JL, Brotman RM, et al. Vaginal biogenic amines: biomarkers of bacterial vaginosis or precursors to vaginal dysbiosis?. Front Physiol. 2015;6:253.
- Mitchell C, Fredricks D, Agnew K, Hitti J. Hydrogen-peroxide producing lactobacilli are associated with lower levels of vaginal interleukin-1, independent of bacterial vaginosis. Sex Transm Dis. 2015;42(7):358-363.
- Koumans EH, Sternberg M, Bruce C, et al. The prevalence of bacterial vaginosis in the United States, 2001-2004: associations with symptoms, sexual behaviors, and reproductive health. Sex Transm Dis. 2007;34(11):864-869.
- Allsworth JE, Peipert JF. Prevalence of bacterial vaginosis: 2001-2004 National Health and Nutrition Examination Survey Data. Obstet Gynecol. 2007;109(1):114-120.
- CDC. Bacterial Vaginosis (BV) Statistics. Prevalence. Page last reviewed December 17. 2015. cdc.gov/std/bv/stats.htm
- Marrazzo JM, Thomas KK, Fiedler TL, et al. Relationship of specific vaginal bacteria and bacterial vaginosis treatment failure in women who have sex with women. Ann Intern Med. 2008;149(1):20-28.
- Marrazzo JM, Thomas KK, Agnew K, Ringwood K. Prevalence and risks for bacterial vaginosis in women who have sex with women. Sex Transm Dis. 2010;37(5):335-339.
- Marrazzo JM, Koutsky LA, Eschenbach DA, et al. Characterization of vaginal flora and bacterial vaginosis
in women who have sex with women. J Infect Dis. 2002;185(9):1307-1313. - Cherpes TL, Meyn LA, Krohn MA, et al. Association between acquisition of herpes simplex virus type 2 in women and bacterial vaginosis. Clin Infect Dis. 2003;37(3):319-325.
- Balkus JE, Richardson BA, Rabe LK, et al. Bacterial vaginosis and the risk of trichomonas vaginalis acquisition among HIV-1-negative women. Sex Transm Dis. 2014;41(2):123-128.
- Ness RB, Kip KE, Hillier SL, et al. A cluster analysis of bacterial vaginosis–associated microflora and pelvic inflammatory disease. Am J Epidemiol. 2005;162(6):585-590.
- Cohen CR, Lingappa JR, Baeten JM, et al. Bacterial vaginosis associated with increased risk of female-to-male HIV-1 transmission: a prospective cohort analysis among African couples. PLoS Med. 2012;9(6):e1001251.
- Low N, Chersich MF, Schmidlin K, et al. Intravaginal practices, bacterial vaginosis, and HIV infection in women: individual participant data meta-analysis. PLoS Med. 2011;8(2):e1000416.
- Brotman RM, Klebanoff MA, Nansel TR, et al. Bacterial vaginosis assessed by gram stain and diminished colonization resistance to incident gonococcal, chlamydial, and trichomonal genital infection. J Infect Dis. 2010;202(12):1907-1915.
- Aghaizu A, Reid F, Kerry S, et al. Frequency and risk factors for incident and redetected Chlamydia trachomatis infection in sexually active, young, multi-ethnic women: a community based cohort study. Sex Transm Infect. 2014;90(7):524-528.
- King CC, Jamieson DJ, Wiener J, et al. Bacterial vaginosis and the natural history of human papillomavirus. Infect Dis Obstet Gynecol. 2011;2011:319460.
- Mitchell C, Moreira C, Fredricks D, et al. Detection of fastidious vaginal bacteria in women with HIV infection and bacterial vaginosis. Infect Dis Obstet Gynecol. 2009;2009:236919.
- Payne SC, Cromer PR, Stanek MK, Palmer AA. Evidence of African‐American women’s frustrations with chronic recurrent bacterial vaginosis. J Am Acad Nurse Pract. 2010;22(2):101-108.
- Faught BM, Dickson RB, Markvicka T. Assessing the Understanding, Impact, and Treatment of Bacterial Vaginosis: Results from Patient and NP/PA Surveys. Presented at: National Association of Nurse Practitioners in Women’s Health Annual Conference; October 2018; San Antonio, Texas.
- Bilardi JE, Walker SM, Temple-Smith MJ, et al. Women view key sexual behaviours as the trigger for the on-set and recurrence of bacterial vaginosis. PloS One. 2017;12(3):e0173637.
- Machado A, Jefferson KK, Cerca N. Interactions between Lactobacillus crispatus and bacterial vaginosis (BV)-associated bacterial species in initial attachment and biofilm formation. Int J Molec Sci. 2013;14(6):12004-12012.
- Ferris DG, Francis SL, Dickman ED, et al. Variability of vaginal pH determination by patients and clinicians. J Am Board Fam Med. 2006;19(4):368-373.
- Bradshaw CS, Sobel JD. Current treatment of bacterial vaginosis—limitations and need for innovation. J Infect Dis. 2016;214(suppl 1):S14-S20.
- Chavoustie SE, Eder SE, Koltun WD, et al. Experts explore the state of bacterial vaginosis and the unmet needs facing women and providers. Int J Gynecol Obstet. 2017;137(2):107-109.
- Gallo MF, Warner L, King CC, et al. Association between semen exposure and incident bacterial vaginosis. Infect Dis Obstet Gynecol. 2011;2011:842652.