In January 2020, the first confirmed case of Covid-19 infection was diagnosed in the United States. As of the end of June 2021, approximately 33,448,524 people in the US alone have been diagnosed with Covid-19 and an estimated 601,573 people have died from complications.1 Survivors include those who were hospitalized for life-threatening or serious illness, those who had mild-to-moderate symptoms managed outside the hospital, and those who were asymptomatic.
The sequelae of Covid-19 beyond the acute phase of infection are becoming increasingly evident as data and clinical experience accrue over time. Physical and psychological complications from prolonged illness and hospitalization may be enduring or appear as late manifestations. Individuals who were determined to have had asymptomatic infection or who experienced mild acute illness are also reporting persistent or newly emerging symptoms.2–4 The healthcare needs of those who have had Covid-19 will continue for the foreseeable future. Healthcare providers in primary care settings have a key role in recognizing and evaluating ongoing or new post-Covid symptoms. Some symptoms may require immediate intervention, some require interdisciplinary collaboration, and some may be addressed through monitoring and implementation of self-care strategies.
Post-Covid terminology, causes, symptoms
The Centers for Disease Control and Prevention (CDC) uses the term post-Covid conditions to refer to the wide range of physical and mental consequences present for 4 or more weeks after onset of Covid-19 infection.3 Other terminology and definitions used include post-acute Covid for symptoms that persist beyond 3 weeks and chronic post-Covid syndrome when symptoms persist to 12 weeks or beyond.4 “Long Covid” and “long-haul Covid” are common terms used to describe the signs and symptoms that continue or develop after acute Covid-19 infection.5,6
The causes for post-Covid conditions are not completely understood and are likely attributable to different underlying processes. Possible etiologies include: virus-specific pathophysiologic changes; immunologic aberrations and inflammatory damage in response to the acute infection; and expected physical and mental sequelae of post-critical illness such as physical deconditioning and post-traumatic psychological stress.3,7
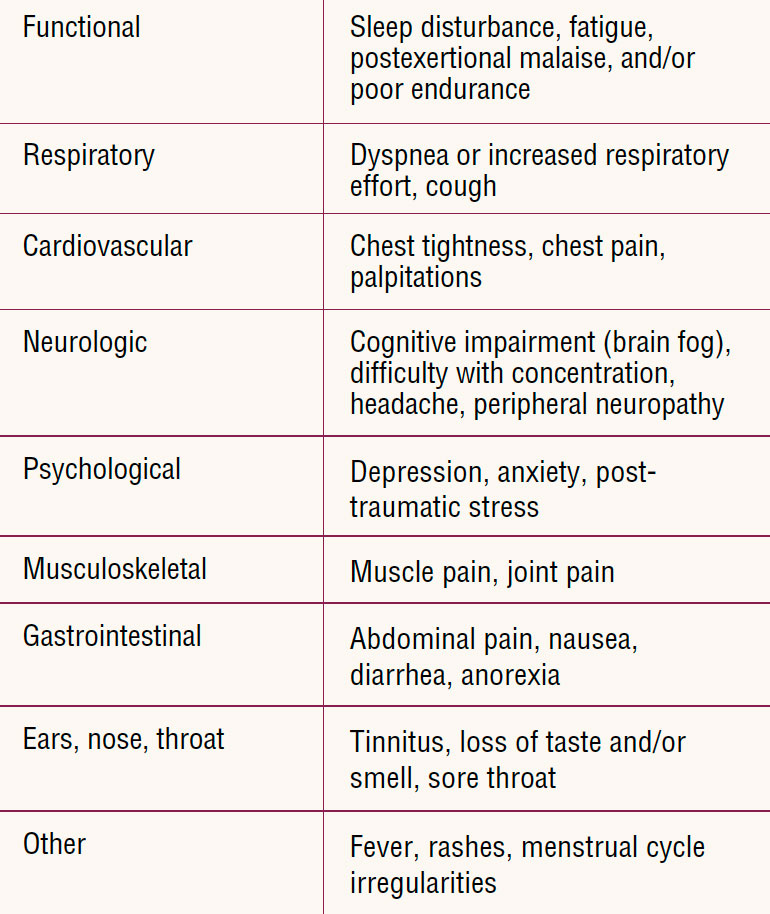
Post-Covid symptoms are reported not only by patients who experienced a severe course of infection but also by individuals after mildly acute illness or an initially asymptomatic infection.3 Just as the etiologies vary, so do symptoms. Almost every body system can be involved, but most prominently these include respiratory, cardiovascular, neurologic, and musculoskeletal systems. Psychological symptoms of anxiety and depression are also common. The Table lists some of the most commonly reported symptoms. Multiple studies and survivor support group surveys are showing that daily functioning and quality of life are negatively impacted by persistent post-Covid symptoms.5–8
Table. Common post-Covid symptoms2,3,5–7
The CDC and the United Kingdom National Institute for Health and Care Excellence (NICE) have each developed guidance documents on evaluating and caring for patients with post-Covid conditions.3,6 Both documents are based on currently available evidence and medical expert opinion. The CDC and NICE note that treatment guidelines and practices can be expected to continue to evolve with increasing knowledge and evidence.3,6
Evaluation
Post-Covid conditions can impact an individual’s ability to perform usual daily activities including self-care, work, school, and interactions with family. Sense of well-being and quality of life can decrease significantly. A holistic, individualized plan of care for each patient starts with recognizing and evaluating symptoms as well as assessing how their life is being affected. A trauma-informed approach is recommended. Especially for those who experienced a potentially life-threatening illness, prolonged social isolation, and long or complicated disease course, there can be significant psychological and emotional consequences.6 Notably, symptoms of post-traumatic stress disorder (PTSD) have been reported in approximately 30% of patients with Covid-19 requiring hospitalization and may manifest early during acute infection or months later.7
Patterns for the onset of post-Covid conditions include but are not limited to symptoms that began at the time of acute illness and have persisted, new onset of symptoms following asymptomatic disease or a period of acute symptom remission, or a combination of persistent symptoms with the addition of new symptoms over time. Individuals can have wide-ranging and fluctuating symptoms.3,6
Most post-Covid conditions can be diagnosed clinically based on patient history and physical examination findings. The health history should be comprehensive so as not to miss any significant findings. The patient’s history regarding suspected or confirmed acute Covid-19 infection; nature, duration, and severity of symptoms during acute infection; complications; treatment; and the timing and duration of current symptoms is essential. The medical history should include assessment of existing conditions that could impact the severity of Covid-19 disease. Assessment of any change in financial, employment, and housing status that could affect needed resources for recovery is relevant. Of utmost importance is a discussion on how the individual’s daily activities, sense of well-being, and quality of life have been affected by ongoing symptoms.3,6
Because post-Covid conditions can involve multiple organ systems, a thorough physical examination should be completed, including vital signs, pulse oximetry, body mass index, and a head-to-toe body systems examination. If the patient has respiratory or cardiovascular symptoms or fatigue, ambulatory pulse-oximetry should be considered to assess for activity-related oxygen desaturation. Further, orthostatic vital signs (supine first, then again sitting or standing) need to be evaluated to assess for orthostatic (postural) hypotension if the patient reports postural symptoms such as palpitations or dizziness.3,6
Laboratory testing should be guided by findings from the patient history and physical examination. Covid-19 viral or antibody tests are not necessary to establish a diagnosis of post-Covid conditions. In some cases, no testing is needed.3,4,6 A basic panel of laboratory tests might be considered (eg, complete blood count, basic metabolic panel, urinalysis, liver function tests or complete metabolic panel, C-reactive protein, erythrocyte sedimentation rate, ferritin, thyroid function test).3,6 The absence of laboratory-confirmed abnormalities should not lead to dismissing the possible impact of a patient’s symptoms on their daily function. More specialized laboratory and diagnostic tests may be indicated when symptoms persist for 12 weeks or longer or when history and physical examination findings suggest the need.3,6
Immediate referral is required when there are signs or symptoms of acute or life-threatening complications, including but not limited to severe hypoxemia or oxygen desaturation on exercise, severe chest pain, multisystem inflammatory syndrome in children, or severe psychiatric symptoms.3,4,6
Management
Patients whose acute illness led to intensive hospital care and those with organ-specific complications that developed during or after acute illness usually require follow-up with a team of specialists to meet their recovery and rehabilitation needs. Some healthcare systems and hospitals have established post-Covid multidisciplinary care centers. Other communities may use the patient-centered medical home model, with coordination of care among a core group of specialty care providers and support services (eg, occupational therapy, physical therapy, social work).3,6,7
However, many post-Covid symptoms can be managed in the primary care setting and often improve without medical intervention during the first few months after initial infection. Acknowledging patients’ symptoms and the impact on their lives, explaining full recovery may take several weeks, using established symptom management approaches, and emphasizing holistic support are strategies the primary care provider can implement.
Goal setting should address the patient’s main concerns. For most patients with post-Covid symptoms, the goal is to optimize function and quality of life. Modest interim goals should be encouraged. Careful pacing of activities and prioritizing what needs to get done are
important while waiting for improvement in energy levels and breathlessness. A gradual return to exercise as tolerated can be helpful for most patients. Phased-in returns to work or school may be necessary. Counseling on lifestyle components such as nutrition, sleep, and stress reduction is valuable in promoting positive self-care. Recommendations on local support groups or online forums can be provided. Finally, it is important to provide individuals who have experienced financial losses with information on resources available to them.
Follow-up approaches that incorporate telehealth, including phone calls and virtual visits, can be beneficial and might lessen the burden on patients with limited energy or who have other concerns about in-person visits. Patients should be encouraged to keep a record of or use a tracking app to monitor their goals, recovery, and any changes in symptoms. Daily self-monitoring of pulse oximetry may also be helpful for some patients for ongoing assessment as well as reassurance.3,4,6 Patients who feel unable to cope with symptoms, with worsening symptoms, or symptoms that persist more than 12 weeks may need referrals for further evaluation and a comprehensive recovery and rehabilitation plan.
Other considerations
The primary care provider can play a key role in addressing the needs of individuals who have not had Covid-19 or who have had it but with complete physical recovery. They may be experiencing grief and bereavement over lost loved ones. They may have lost jobs when the country implemented regulations on social distancing. A growing number of studies have reported the general population experiencing significant psychological symptoms related to intense stress.5 In particular, healthcare and other frontline workers are suffering from secondary traumatic stress and PTSD.4,9,10 Management strategies described for those with post-Covid symptoms may be helpful for these individuals also.
Conclusion
We are hopefully going to see a continuing decline in Covid-19 cases and deaths. As well, we are looking forward to a return to prepandemic levels of social interaction and a reduction in financial and other Covid-related stressors. Healthcare providers in primary care settings will, at least for the near future, continue to be at the forefront in recognizing and evaluating ongoing or new post-Covid symptoms. Holistic, individualized care will help patients fully recover and regain their sense of well-being.
Beth Kelsey is the Director of Publications for the National Association of Nurse Practitioners in Women’s Health in Washington, DC, and the Editor-in-Chief of this journal. The author has no actual or potential conflicts of interest in relation to the contents of this article.
References
Centers for Disease Control and Prevention. COVID data tracker. http://covid.cdc.gov/covid-data-tracker.
Tenforde MW, Kim SS, Lindsell CJ, et al. Symptom duration and risk factors for delayed return to usual health among outpatients with COVID-19 in a multistate health care systems network—United States, March–June 2020. MMWR Morb Mortal Wkly Rep. 2020;69(30):993-998.
Centers for Disease Control and Prevention. Evaluating and caring for patients with post-COVID conditions: interim guidance. June 14, 2021. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/post-covid-index.html.
Greenhalgh T, Knight M, A’Court C, et al. Management of post-acute covid-19 in primary care. BMJ. 2020;370:m3026.
Orrù G, Bertelloni D, Diolaiuti F, et al. Long-COVID syndrome? A study on the persistence of neurological, psychological and physiological symptoms. Healthcare (Basel). 2021;9(5):575.
National Institute for Health and Care Excellence. COVID-19 rapid guideline: managing the long-term effects of COVID-19. December 18, 2020. https://www.nice.org.uk/guidance/NG188.
Nalbandian A, Sehgal K, Gupta A, et al. Post-acute COVID-19 syndrome. Nat Med. 2021;27(4):601-615.
Jacobs LG, Paleoudis EG, Lesky-Di Bari D, et al. Persistence of symptoms and quality of life at 35 days after hospitalization for COVID-19 infection. PloSOne. 2020;15(12):e0243882.
Orrù G, Marzetti F, Conversano C, et al. Secondary traumatic stress and burnout in healthcare workers during COVID-19 outbreak. Int J Environ Res Public Health. 2021;18(1):337.
Bryant-Genevier J, Rao CY, Lopes-Cardozo B, et al. Symptoms of depression, anxiety, post-traumatic stress disorder, and suicidal ideation among state, tribal, local, and territorial public health workers during the COVID-19 pandemic—United States, March–April 2021. MMWR. June 25, 2021.

